Can data on discharge times help us to improve hospital flow?
For some time, policy-makers have urged hospitals to discharge patients earlier in the day, ideally before noon, as a means of improving hospital flow. This analysis assesses whether the commissioning datasets used to monitor hospital activity are capable of providing useful and reliable information on this issue. Having established the coverage and credibility of the data, we describe the admission and discharge profile of patients over the course of the day and consider opportunities to improve patient flow.
Key Messages
Until recently, the commissioning dataset for admitted patient care, contained information about the date of a patient’s discharge from hospital, but not the time. This shortcoming was rectified several years ago, and completion rates of discharge times have been steadily increasing ever since.
In March 2025, 86.6% of records for elective and emergency hospital spells in England contained a valid discharge time. In a large subset of hospital trusts, recording of discharge times has been virtually complete since 2022.
The proportion of patients who are discharged in the morning has been increasing slowly since 2022. In 2024/25, 1 in 6 patients were discharged before noon. Some providers manage to discharge 1 in every 4 patients before noon.
Long waits in A&E are often attributed to a shortage of free beds within hospitals. Our analysis shows that this shortage is greatest in early afternoon. This is because for each hour until 1pm the number of admissions exceeds the number of discharges.
Increasing the number of discharges before noon could therefore reduce this peak and the pressure on beds. The relationship between a hospital’s daily discharge profile and the flow of patients in its emergency departments is likely to be complex and dynamic. More detailed analysis would be required to test empirically, whether increasing the rate of morning discharges leads to improvements in ED flow.
Further work is required to understand the casemix factors that influence the likelihood that a patient will be discharged in the morning. This information is required before providers could be fairly compared in terms of the proportion of patients discharged before noon.
Policy-makers should resist the temptation to create a ‘discharge before noon’ performance target for hospital trusts. This would lead to unintended consequences that may outweigh any gains.
Pressure on hospital beds
Do we have enough hospital beds to deal with patient demand? This question must feature heavily in the list of concerns of health ministers and hospital CEOs. Excessive pressure on beds can lead to poor use of resources, poor patient experience, and poor patient outcomes. The pressure creates problems that propagate upstream into emergency departments, ambulance services, and elective pathways, and downstream to community services and social care. Although a constant concern, the pressure on beds does vary in strength. Average inpatient occupancy rates crept up slowly from around 85% in 2010 to 90% in 2020, reducing abruptly during the COVID-19 pandemic, before stabilising at around 91% in recent years. There are also regular seasonal patterns, with occupancy rates typically 2 or 3 percentage points higher in the winter than the summer. And there are regular daily patterns in occupancy rates too.
The solutions offered to this problem depend on the timescale in mind. Taking the long-term view, the solutions focus on improving population health, redesigning community and primary care, or increasing bed stock to levels closer to those seen in other European countries. When the focus is pressure in the winter then healthcare systems consider diverting patients to other settings, or rescheduling elective activity. One of the solutions offered when taking an in-day perspective on bed pressures, is to increase the proportion of patients who are discharged earlier in the day. This idea is often simplified to a single metric to be optimised: the proportion of patients who are discharged before noon.
Discharge before noon
Although ‘discharge before noon’ receives a lot of attention in the narrative sections of improvement guides, quantitative performance assessments rarely feature. The constraint here is data. To understand the in-day profile of inpatient discharges, or to calculate the proportion of patients discharged before noon, we need data on the time of discharge for all hospital stays. Hospital trusts record this information as a matter of course, but until recently, it hasn't flowed into the standard commissioning datasets. The 'discharge time' field was added a few years ago, however, and although not mandatory, trust compliance with this new submission expectation has been slowly improving.
In this analysis we explore whether coverage and quality of this new 'discharge time' field is sufficient to allow us to gain an understanding of the pattern of discharges over the course of the day, the proportion of patients who are discharged before noon, and the implications of this information for the operational management of hospitals. Further details of the methods and data sources used are available in a working paper. The work was funded and helpfully guided by the Health Foundation.
Can we measure 'discharge before noon'?
In an ideal world, every record of a completed inpatient stay in the commissioning datasets, would include a valid discharge time. In fact, in March 2025, valid discharge times were assigned to 86.6% of elective and emergency spells and this proportion has been steadily creeping up for several years. But there is a large subset of acute hospital trusts (n = 136 or 78%) that recorded discharge times for more than 99% of spells over the three-year period from April 2022 to March 2025. We base the remaining analysis in this blog, on the data from these trusts and over this period, since this reduces the uncertainty in our analysis. And because this subset of trusts is large and diverse and delivered more than three quarters of all acute hospital spells, we can reasonably infer that the results will not differ substantially from those of England as a whole.
Recording practices vary somewhat between and within trusts. Some records include discharge times rounded to the nearest minute, in other cases, discharge times appear to be rounded to the nearest 5, 15, 30 minutes or even to the nearest hour. To accommodate this variation in our analysis, we report results by hour only.
When are patients discharged?
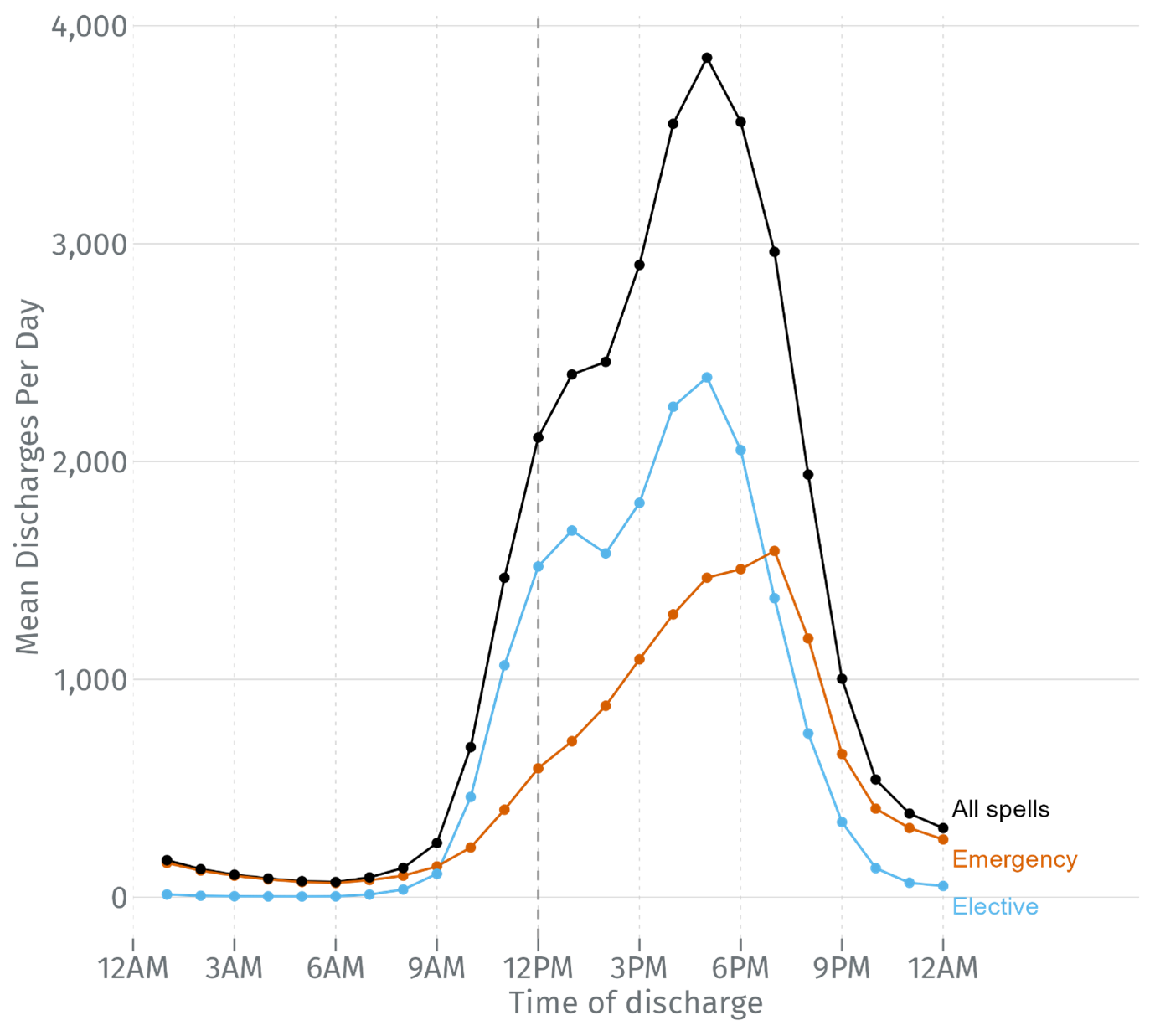
Figure 1 shows how often patients are discharged at each hour of the day. As we might expect, the number of patients who are discharged between midnight and 8am is negligible. The number of discharges increases rapidly during the day, slowing at lunchtime, before increasing again and reaching a peak in late afternoon. The period between 4 and 5pm was the modal discharge hour in each of the three years we examined.
Figure 1: Average daily frequency of discharge times by hour of day | Subset of 136 NHS Trusts in England | April 2022 – March 2025 | Elective and emergency spells only
The modal discharge time for elective patients is also 4-5pm, two hours ahead of the modal discharge time for emergency patients.
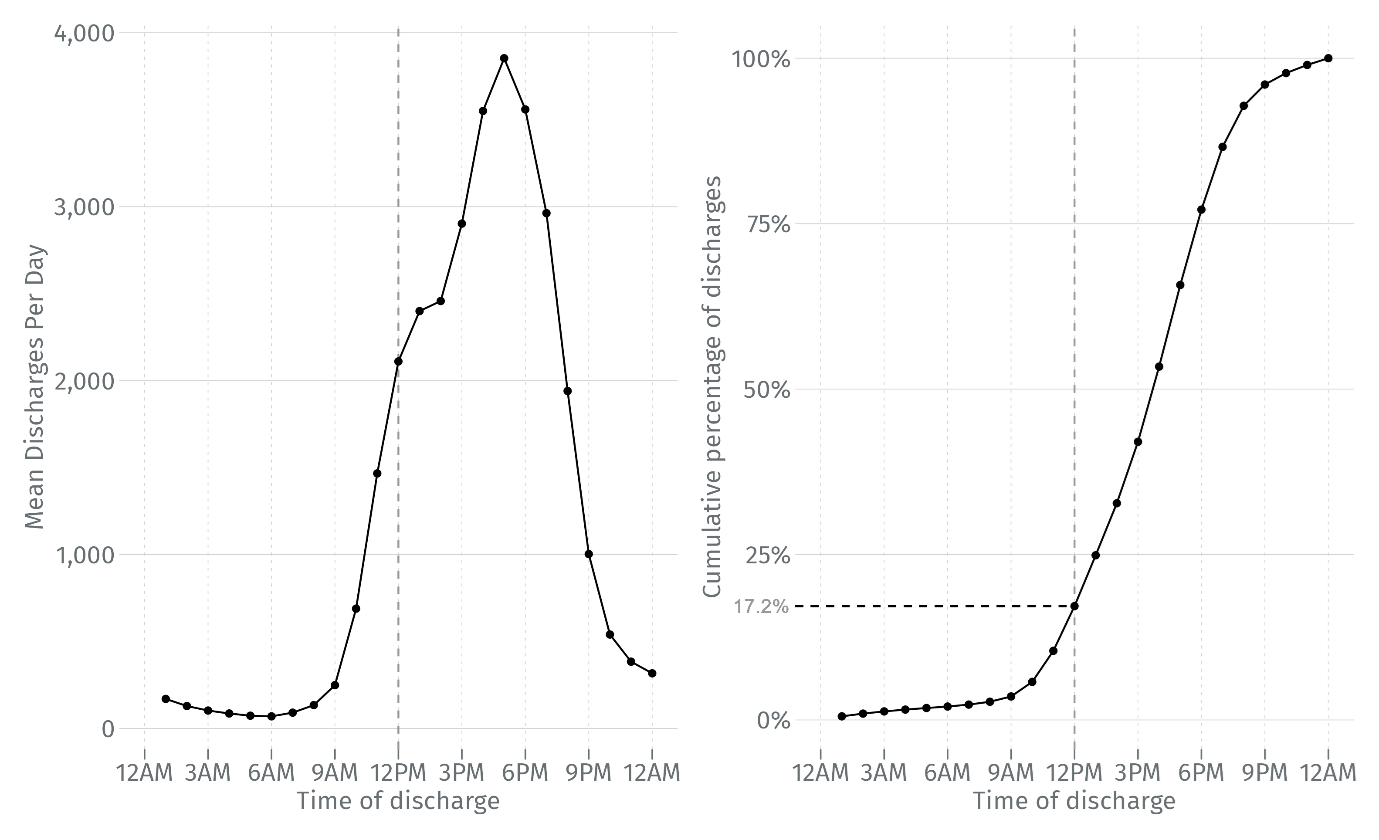
Figure 2 demonstrates another way to view this data. The left-hand panel repeats figure 1. In the right-hand panel, we show the cumulative frequency of discharges over the course of the day. This shows that roughly 17% of patients (1 in every 6) in the trusts that we studied, are discharged before noon, and that half of all patients that will be discharged on any given day are still in hospital at 4pm.
Figure 2: Average daily frequency (left) and cumulative frequency (right) of discharge times by hour of day | Subset of 136 NHS Trusts in England | April 2022 – March 2025 | Elective and emergency spells only
Bed occupancy increases during the morning and early afternoon
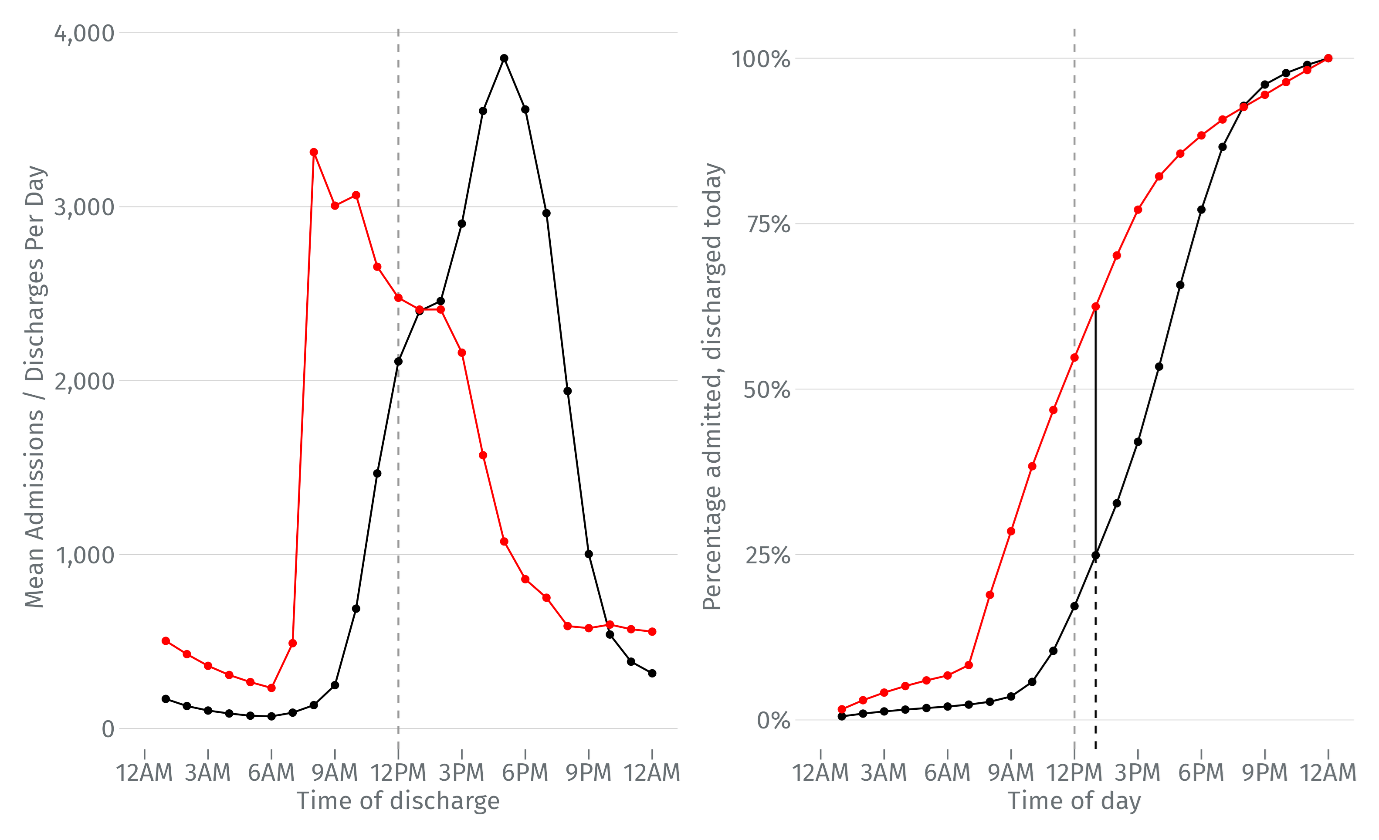
The number of occupied hospital beds increases when the number of patients being admitted exceeds the number of patients being discharged. Figure 3 below sets the daily profile of admissions to hospital beds alongside the profile of discharges. It shows that the rate of admissions substantially outstrips the rate of discharges in the morning. The pivot point occurs around 1pm.
Figure 3: Average daily frequency (left) and cumulative frequency (right) of admission (red) and discharge times (black) by hour of day | Subset of 136 NHS Trusts in England | April 2022 – March 2025 | Elective and emergency spells only
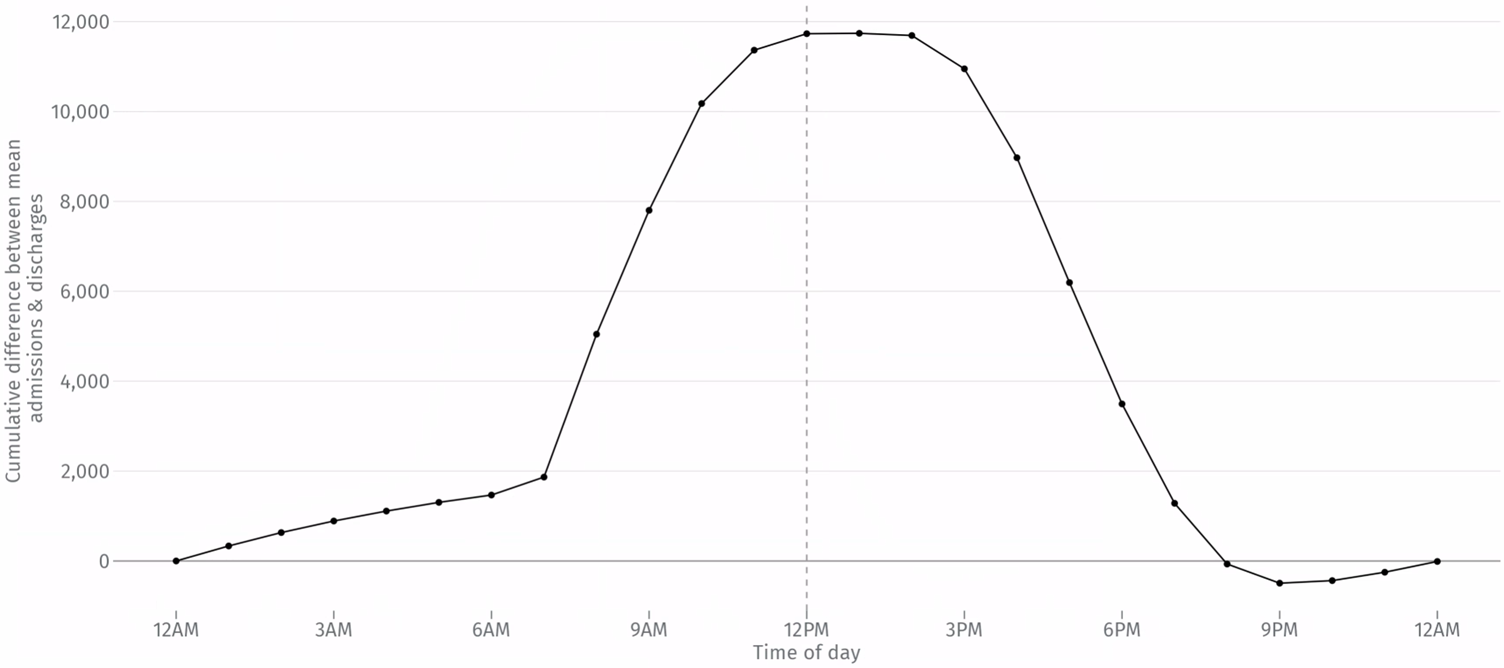
Figure 4 shows the net impact of these admission and discharge patterns on the daily cycle of bed occupancy. Occupancy rates increase slowly throughout the night and early morning, before rising sharply between 8am and 11am. Occupancy peaks at 1pm but is sustained at high levels until around 4pm. By 7pm levels have returned to those seen 12 hours earlier.
Figure 4: Average inpatient occupancy by hour of day, relative to midnight | Subset of 136 NHS Trusts in England | April 2022 – March 2025 | Elective and emergency spells only
Earlier discharges would reduce the pressure on beds
Variation in bed use over the course of the day, resulting from the mismatch between the admission and discharge profile, can be thought of as a source of inefficiency. If the number of patients varies systematically over the day, then hospitals need to accommodate the number of patients at the peak, and leave expensive beds unoccupied at other times. Hospitals organise staffing rotas and use day-only beds to mitigate these inefficiencies, but might it be possible to better align the admission and discharge profiles to reduce in-day fluctuations in demand at source? This is the idea that underpins policies variously known as ‘early day discharge’, ‘discharge before noon’, and ‘home before lunch’.
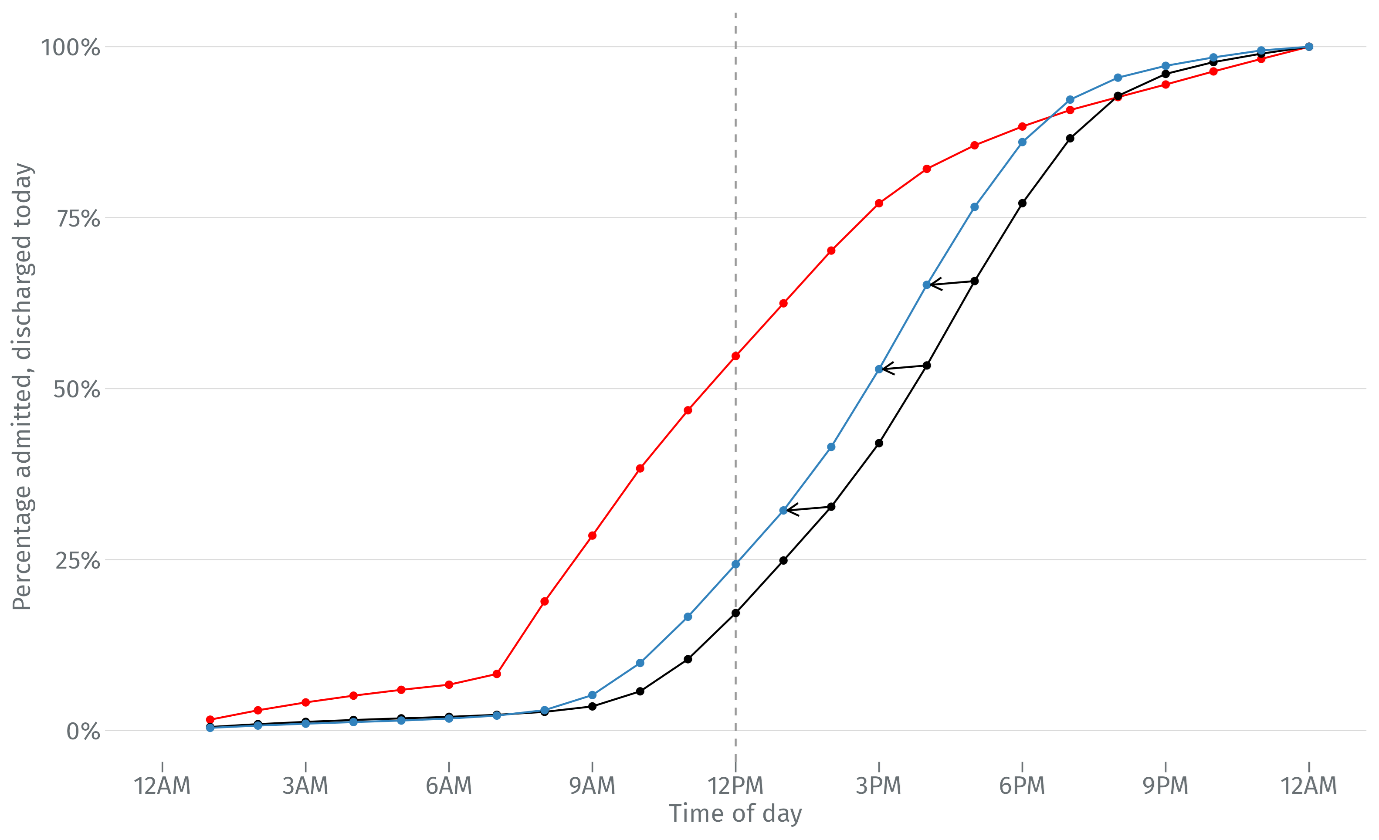
In theory, even modest shifts in the discharge profile can free up a considerable number of beds. To illustrate this effect, we estimated the number of beds that would be released if we shifted the cumulative discharge curve, 1 hour to the left, as shown in figure 5, reducing the gap between the admission and discharge profile.
Figure 5: Shifting the discharge curve (black) by 1 hour (blue) to close the gap to the admission curve (red)
The effect of even this modest shift in the discharge profile is significant. 1 in 4 patients (25%) would be discharged before noon, an additional 2,230 patients on an average day, in our sample of 136 trusts. If we assume this effect would be present in all trusts in England and factor in the number of available beds, then this would amount to an average 2.4 percentage point reduction in bed occupancy at that highly pressurised time of day. Table 1 presents these effects at other times of the day.
Table 1: Modelled number and percentage of beds freed up at selected times on an average day if patients were discharged 1 hour earlier* | England | 2024/25
| Time of day | Number of beds freed up | % of beds freed up |
| 10am | 1,670 | 1.4% |
| 12pm | 2,870 | 2.4% |
| 2pm | 3,510 | 3.0% |
| 4pm | 4,740 | 4.0% |
| 6pm | 3,590 | 3.0% |
* assuming no change in the admission time profile | changes are relative to the current discharge profile
Peak occupancy, which occurs at around 1pm, would be reduced by 2.5%.
In reality however, it is unlikely that these modelled bed occupancy reductions would come to pass. As beds are released, many would be rapidly filled with patients queuing in emergency departments: an inter-day version of Roemer’s Law. But this in itself, is a positive effect, reducing boarding times in Emergency Departments, and improving patient experience, outcomes, and flow.
Whilst we have modelled what appears to be a modest shift in the discharge profile, the cost and effort required to deliver this shift may not be insignificant.
Trends and variation in early day discharges
The increased coverage of the discharge time field in the commissioning datasets, allows us to explore trends in the proportion of patients who are discharged before noon, and variation between hospital trusts, and patient subgroups. For the purposes of the subsequent analysis, we count early day discharges as those taking place between 6am and noon.
The proportion of patients who experience an early day discharge has increased slowly over the past few years, from 14.8% in April 2022 to 15.5% in March 2025. Seasonal patterns are modest, with slightly lower rates seen in May and September. Patients discharged at the weekend are slightly more likely to leave hospital before noon.
Patients who were admitted the day before are substantially more likely to leave hospital before noon, but once a patient has been in hospital for 3 or more nights, their chance of leaving hospital before noon falls back to the average. Some patients are admitted and discharged on the same day. Interpreting the early day discharge rate for these cases is challenging because many will have been admitted after lunch. As it happens however, the proportion of same-day patients who are discharged before noon is similar to the rate observed in those that have been in hospital for 3 or more days.
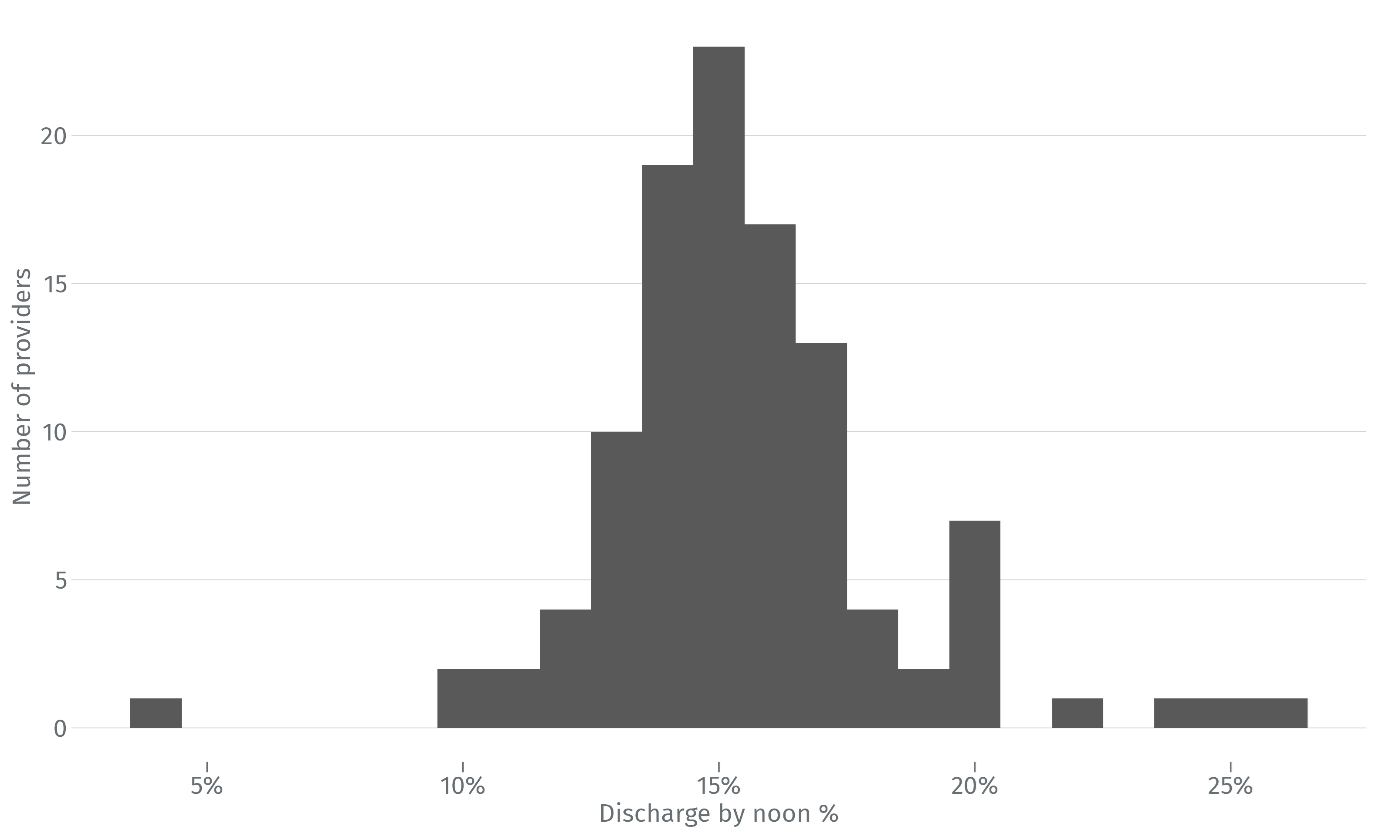
Figure 6 illustrates how the rate of early day discharge varies between hospital trusts. Most trusts discharge between 13% and 17% of patients between 6am and noon. A small number of trusts, however, achieve rates around 25%. Our earlier analysis indicates that a trust performing at the average, could achieve this rate of discharge before noon, by shifting the discharge curve by one hour.
This variation between providers may reflect differences in discharge practices, or differences in the mix of patients that providers treat, or the procedures that they carry out. Controlling for these casemix factors would be required if providers are to be fairly and meaningfully compared in terms of early day discharge rates.
Figure 6: The proportion of patients discharged between 6am and 12pm, by selected hospital trusts and excluding those with <1000 spells | April 2022 – March 2025
Impact on Emergency Department flow
The case for increasing early day discharges, is often made in terms of the opportunity to address long-standing problems with the flow of patients through emergency departments. Patient arrivals into emergency departments exhibit a strong daily pattern. A small but not insignificant number arrive during the night, before a rapid increase over the course of the morning, with sustained high levels between noon and 6pm. Around 1 in every 4 of these patients are admitted to hospital. The emergency care dataset includes information about the timing of the decision to admit a patient. Although not always complete, this field contains useful insights. The number of decisions to admit rises steadily from around 8am to 5pm, and then tails off slowly during the evening and nighttime. This means that many decisions to admit are taken when bed occupancy is at its daily peak. The consequence is that sick patients can spend many hours on a trolley in the emergency department, waiting for a bed to become available. This is bad for patients, and for the efficient operation of emergency departments.
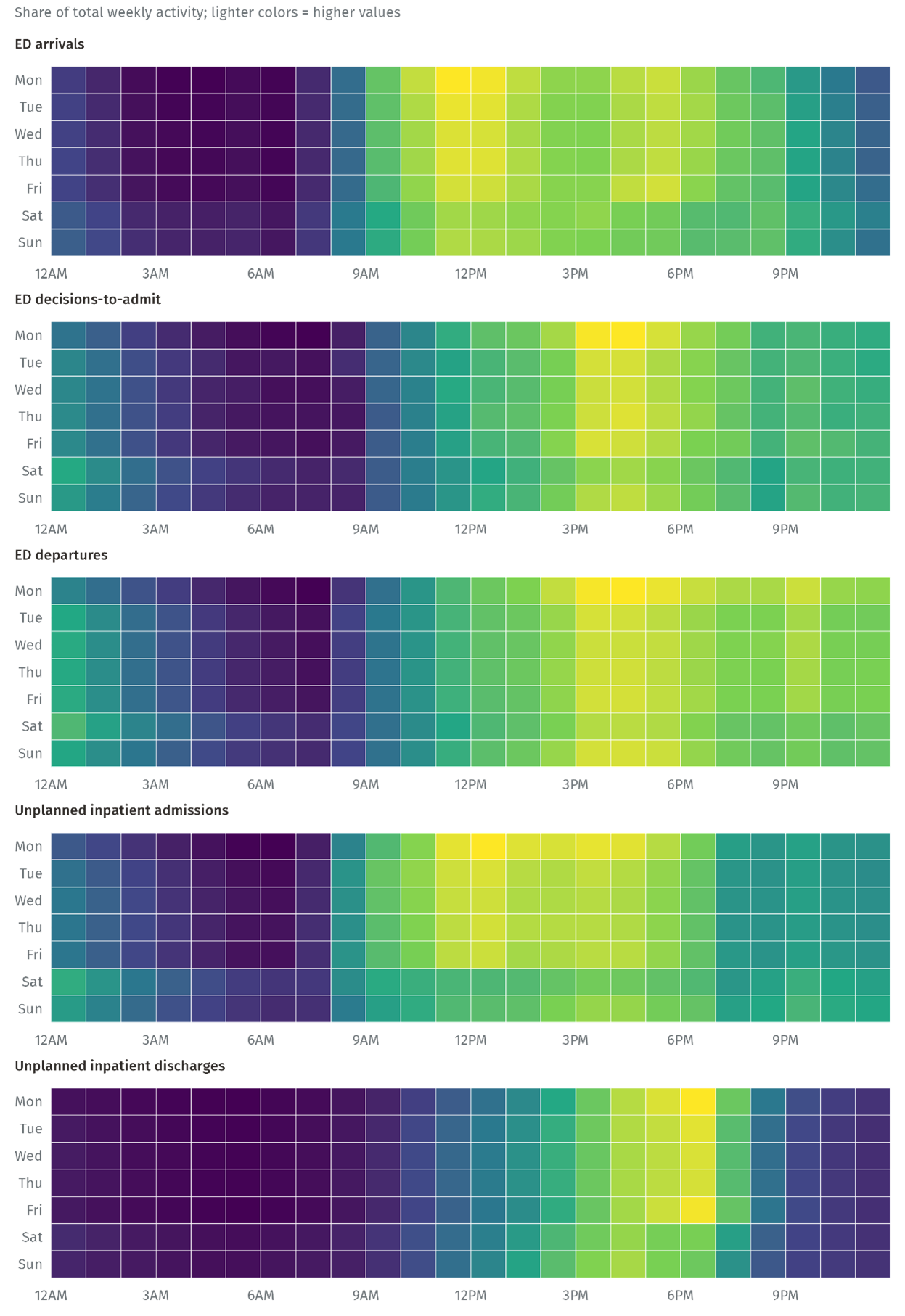
Figure 7 shows this weekly pattern of arrivals and departures into emergency departments and admission and discharge of emergency patients in and out of hospital beds. Whilst ED arrivals and emergency admissions are broadly distributed over the week, the discharge of emergency patients from hospital beds is highly concentrated in the early evenings of weekdays.
Figure 7: Heat maps showing the relative frequency of ED arrivals, decisions-to-admit and departures, and emergency inpatient admissions and discharges, by hour of day and day of week | Selected provider trusts | April 2024 to March 2025
Given the variation between provider trusts in rates of early day discharge, we might perhaps expect those providers that discharge more patients before noon, to be those that perform better against the 4-hour emergency department target, or to have lower boarding times. Whilst a theoretically sound argument, detecting this effect would likely require complex modelling that would take account of all other factors known to influence the flow of patients through emergency departments. Such modelling is beyond the scope of this analysis. A visual inspection of the relationships between these variables, however, suggests there is no clear and simple association. Further analysis to draw out the contribution of early day discharges to emergency department flow is warranted.
In this analysis we have not distinguished between the types of beds that patients have been discharged from. It is likely that discharges from some beds, for example in acute medical units, have a greater impact on emergency department flow than others. This information is available to hospital trusts and was added to the commissioning datasets a few years ago. Much as we have done here for the ‘discharge time’ field, there may be value to exploring the completeness and consistency of this ward type field.
Beware Goodhart’s Law
When a metric becomes part of a consequential performance management regime, then busy staff responsible for delivering performance improvements, must find efficient ways to do so. Unfortunately, the most efficient means of improving reported performance is often to contort recording and operational practices in ways that undermine the original intention of the metric. One way in which this manifests is as a threshold effect. When systems are incentivised to achieve something relative to a threshold (a time for example), then staff working in the system tend to spend a disproportionate amount of effort, on those cases that would otherwise fall just beyond the threshold.
If the proportion of patients 'discharged before noon' becomes a target, then abstracted performance reports may draw no distinction between a discharge that takes place five minutes after noon, and one that takes place at five minutes before midnight. Worse still, a discharge at 11:00 tomorrow might be seen as preferable to a discharge at 13:00 today. Indeed this may be why the evidence from the US, where discharge before noon has received a lot of attention, remains mixed.
Whilst the concept of early day discharges is widely known and understood within provider trusts we saw no clear evidence of widespread efforts to distort discharge timings to maximise the number of patients who leave hospital just before noon. System designers and regulators should take care not to lean too heavily on this metric through performance management mechanisms, if they want to retain its statistical value. As Goodhart’s Law states, “When a measure becomes a target, it ceases to be a good measure.”
Conclusion
In this analysis, we have shown that the discharge time field in the commissioning datasets, has achieved a level of maturity such that it can be used, with care, to understand the daily profile of hospital discharges, and to monitor the proportion of patients who are discharged before noon.
In 2024/25, only 1 in 6 patients were discharged before noon. The rate of early day discharges is increasing, if slowly. There is a modest degree of variation between providers in terms of the proportion of early day discharges. Further work is required to understand this variation and to quantify its impact on flow through emergency departments.
In theory, shifting the distribution of discharges by one hour, would mean that 1 in 4 patients would be discharged before noon, freeing up a significant number of beds at the busiest time of the day. A small number of trusts already deliver this rate of discharge before noon.