In this long-read, which first appeared in the HSJ, Fraser Battye asks whether focusing on continuity might also improve access to primary care
The NHS has been given the task of simultaneously saving money, shifting care and improving outcomes. Fortunately, it knows what to do. Unfortunately, it is busy forgetting how to do it. And tragically, it may be sabotaging its own efforts.
In approaching this task, relational continuity in primary care (seeing the same GP over time) is one of the safest bets the NHS could make. A recent article in the BMJ, by Dr Luisa Pettigrew and colleagues, reminds us that continuity has been well studied - and that it is associated with:
- Reduced mortality.
- Fewer hospital admissions.
- Fewer visits to the emergency department (ED).
- Improved patient experience.
- Increased clinician satisfaction.
The article could have listed other benefits: including more effective prescribing and more efficient use of general practice itself (better continuity leads to fewer visits). It could even have noted that continuity is chosen by the Royals.
No intervention is harm-free, and these upsides come with downsides. It is, for example, possible to see how continuity may offer fewer opportunities for a second opinion. But if continuity was a drug, the inventor would be rich for many lifetimes to come. Here is an approach with a solid evidence base, that provides highly desirable outcomes, and that the NHS knows how to deliver. No tricky breakthroughs in knowledge or as-yet-unimagined technologies are required.
We just need to keep doing something that we have done for a long time.
And yet…
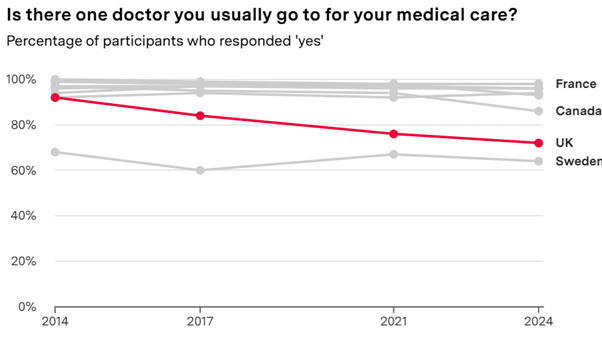
Continuity of care is in decline. The chart below is taken from the Commonwealth Fund 2024 Survey. It shows that in 2014, 92% of UK respondents reported usually going to one doctor for their care; in 2024, the figure was 72%. The chart also shows that continuity did not fall everywhere, and that the UK was an outlier internationally. Both history and experience elsewhere suggest that decline is far from inevitable: it is the result of choices.
It is worth pausing to see what this means. The evidence for continuity’s positive effects is clear. A quick flip of the logic therefore suggests that the recent decline in continuity must mean:
- Increased mortality.
- More hospital admissions.
- More visits to the ED.
- Worse patient experience.
- Decreased clinician satisfaction.
- Increased pressure on primary care appointments.
- Less effective prescribing.
It wouldn’t be trivially easy, but the scale of these effects could be estimated. How many extra ED attendances have resulted? How many extra appointments in primary care? How many GPs leaving the profession? How much money spent on inappropriate prescribing? How much patient harm? How many years of life lost?
And, even without doing the maths, the list above will resonate with everyday experience across the NHS. From this perspective, the decline in continuity looks like an act of self-harm.
What explains the turn away from continuity?
The usual explanation is an emphasis on access – and an apparent trade-off between access to care and continuity of it.
The figures for accessing primary care are grim. The GP Patient survey shows that in 2012, around 80% of people said it was ‘easy’ to get through to their practice by telephone. In 2025, this had fallen to 50%. More historic comparisons are so unflattering as to be darkly funny: in 1959, around half of people in England regarded their GP as a personal friend.
This decline has become politically potent. Access to primary care now polls as the top public priority for the NHS. These concerns have animated a concerted policy and service push to increase access.
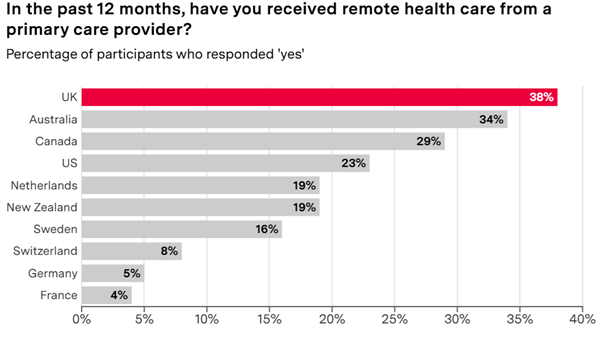
In their BMJ article, Pettigrew and colleagues list a familiar set of interventions and trends, including: the introduction of new roles (e.g. physician assistants), larger practice sizes, stratifying patients by risk, pharmacy first, and increased use of digital access. The Commonwealth Fund survey shows one of the effects of this: the UK is a high user of digital access.
Each of the above approaches are – almost by definition – less well-studied and less certain in their effects than relational continuity. They are all riskier bets. And some – such as risk stratification – look like a busted flush. Furthermore, there seems to be a growing consensus that efforts to increase access are leading to declines in continuity.
There are some types of consultation where speed and convenience of access are, above all else, what matters. I haven’t been to the GP for years: the idea of continuity makes no sense in my case. And what I would need is a quick, easy route in that fits life’s other demands. But should demands of my type be what animates policy? Or could needs like mine be spotted and segmented? Could we seek access for some and continuity for others?
Or is there another way to think about this? Are we assuming a tension that isn’t there?
Could improving continuity also increase access?
The current debate seems to present a flat choice: either more access or better continuity.
In some ways, this is intuitive and true. For example, it is possible to see how having a large practice where any GP could be matched to any patient provides many more appointment options – and so better access – than the same number of GPs dedicated to a specific list of ‘their patients’.
And yet, it is also possible to see how this unravels over time. Following the same example, reductions in continuity lead to declining clinician satisfaction: this would tend towards more part-time working and reduced retention. Reduced continuity also increases demand for appointments: this builds pressure within the practice and drives activity elsewhere in the system. And policy contains its own self-reinforcing feedback loop: problems of access lead to further pushes on access.
Focusing on access may therefore harm both continuity and – over time – access itself. As a 2025 paper in the British Journal of General Practice notes:
“This seems paradoxical. At the time when an individual requests an appointment, there is a trade-off between an immediate appointment with any GP and continuity with a specific GP. But because practices with high continuity have lower demand for appointments, we observe, counterintuitively, that they also tend to have better access.”
Reviewing the evidence, Strategy Unit analysis suggests that there is something in this – and that doing so may also help efforts to reduce health inequalities. And our Head of Research and Policy, Steven Wyatt produced this illustration showing how continuity may - over time - also improve access.
Where next?
Focusing on access may reduce access. But focusing on continuity – which seems in tension with it – may, in the end, improve access. This topic contains apparent paradoxes.
And so it is when thinking about the response.
There is a clear policy direction to shift care and make better use of resources. There are opportunities to improve outcomes and reduce inequalities. There is a workforce crisis and a need to improve GP recruitment and retention. And there is growing evidence that the push on access may be self-defeating.
Even so, it would be an act of bravery to turn away from access and towards continuity. What looks like the safest bet appears to be the hardest one to make.
CC BY-NC-ND 4.0

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.