When we began looking at failure demand in the NHS, I assumed most of our time would be spent in familiar territory: productivity metrics, appointment volumes, activity data, and trends that could be graphed and compared. Failure demand is, after all, usually introduced as an efficiency concept: work created when a system fails to meet need the first time.
But what stayed with me most, from interviews and conversations across the system, was something else entirely.
It was the human work that sits underneath the figures - and how invisible much of that work has become.
Failure demand describes the additional contacts, appointments and activities generated when a person’s need is not met properly first time. A patient who calls back because a referral was never actioned. A carer who spends hours chasing test results that should have been communicated. A person whose condition deteriorates on a waiting list and then needs more complex, more costly care.
None of this reflects new or unavoidable demand. It is work the system has created for itself.
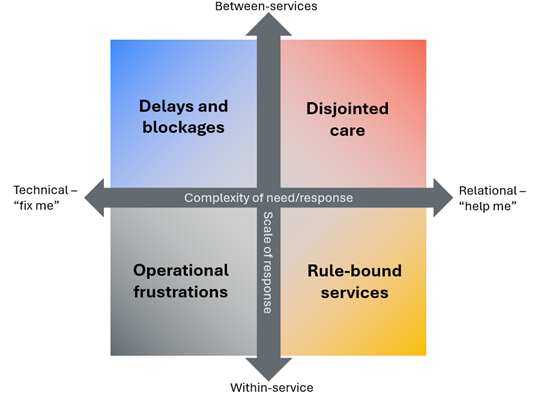
As the project developed, it became clear that lumping all of this together under a single label - “failure demand”- was part of the problem. That led us to develop an exploratory typology, not as a definitive classification, but as a way of making more careful distinctions.
In simple terms, the typology draws attention to two questions.
First, is the interaction primarily transactional - a bounded “fix me” problem that ought to be resolvable with the right process? Or is it relational - a more complex “help me” situation, shaped by context, ongoing need and relationships over time?
Second, does the failure sit within a single service, or does it emerge between services, at the boundaries where responsibility becomes blurred?
These distinctions matter. Repeated appointment booking errors or missing referrals are very different problems from fragmented support for people with complex needs - and they respond to very different improvement approaches. Transactional failures within a service may be amenable to process redesign and quality improvement methods. Relational failures across services raise deeper questions about system design, incentives and how care is coordinated.
This also sharpened the productivity paradox at the heart of the work. In conventional metrics, all activity counts as output, including activity generated by failure demand. A patient who returns because a referral was never actioned generates an appointment that appears productive on paper. Systems with high levels of failure demand can therefore look busy, even efficient, while failing to meet need well.
Seen through this lens, the question is not simply how much work the NHS is doing, but how much of that work exists only because the system couldn’t do something else earlier or differently.
What makes failure demand challenging to discuss is not individual behaviour, but what it reveals about how the system is configured. Thresholds, incentives, hand‑offs and organisational divides interact over time, creating patterns of work that no single team has chosen, but many end up absorbing.
Failure demand is not a problem that can be neatly measured or “solved”. The boundaries are fuzzy, and not all repeat contact is inappropriate. But that ambiguity may be part of its value. Used carefully, failure demand acts as a signal, prompting better questions about why work keeps circling back and what that reveals about unmet need.
If we’re willing to pay attention to failure demand - and what it tells us about unmet need and system design - it may offer a practical route to doing things better.
Taking the conversation further
We’re hosting a webinar (Register here), bringing together perspectives from National Voices, the Association of Ambulance Chief Executives, the Health Foundation and the Strategy Unit. We hope it will offer space to explore what failure demand looks like from different vantage points - and what responding to it might require in practice.
The full report sets out our findings, an exploratory typology of failure demand signals, and recommendations for policymakers, system leaders and researchers. We hope it provides both a lens for reflection and a starting point for action, particularly as the NHS seeks not just to do more, but to do what genuinely adds value.
This work was funded by the Health Foundation, and builds on their long-standing interest in productivity, value and system learning in health and care.