The current coronavirus pandemic has prompted a highly-charged debate in which what is good for health and what is good for the economy are unhelpfully and inaccurately set in opposition to one another. In a novel analysis for the Healthier Futures Academy in the Black Country and West Birmingham, we illustrate the effects that a COVID-driven recession could have on population health, and we frame a discussion about how the NHS, with other local organisations, can more effectively address the causes as well as the effects of ill health.
If we do too little, this virus will go out of control and we will get significant numbers of increased direct and indirect deaths, but if we go too far the other way, then we can cause damage to the economy which can feed through to unemployment,to poverty and to deprivation, all of which have long-term health effects. So we need always to keep these two sides in mind.
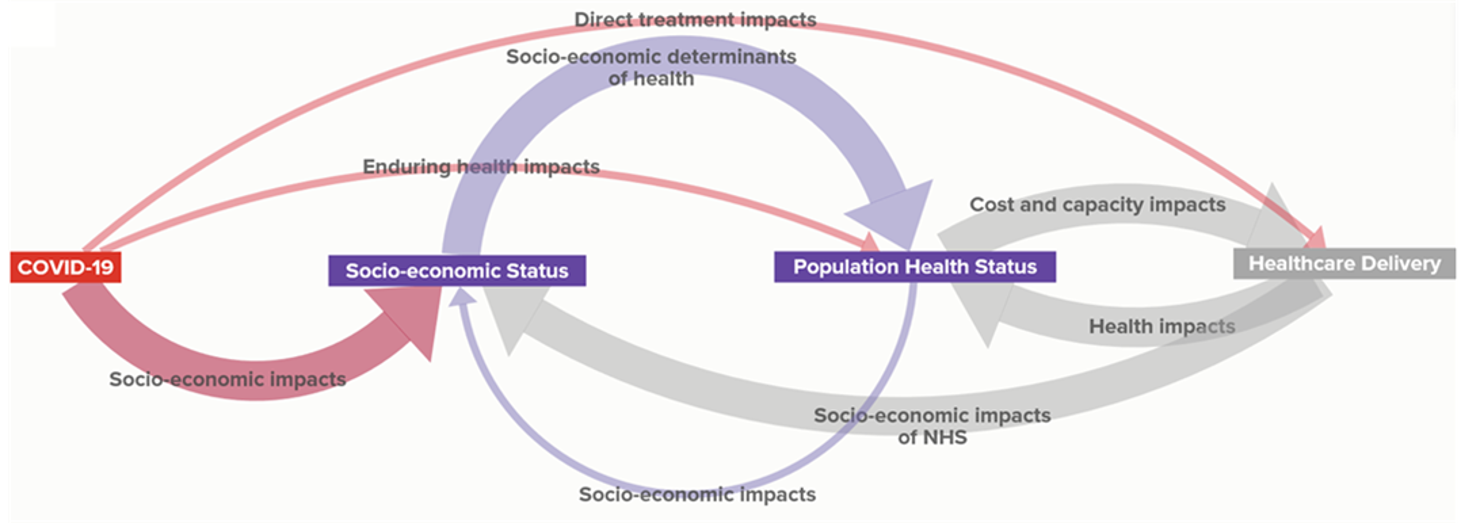
COVID-19 has a 4-fold effect on population health and the provision of healthcare services:
- The direct healthcare impact of the disease itself
- The emerging impact of ‘long-COVID’ in those continuing to live with the effects of the disease.
- The impact of COVID pressures on the diagnosis and treatment of other conditions, such as cancer and heart disease. Data on excess non-COVID deaths in the home bear witness to this.
- The ill-health that will result from the economic recession brought on by COVID-reduction measures.
Each of these impacts are likely to disproportionately affect deprived communities, and the BAME residents within them.
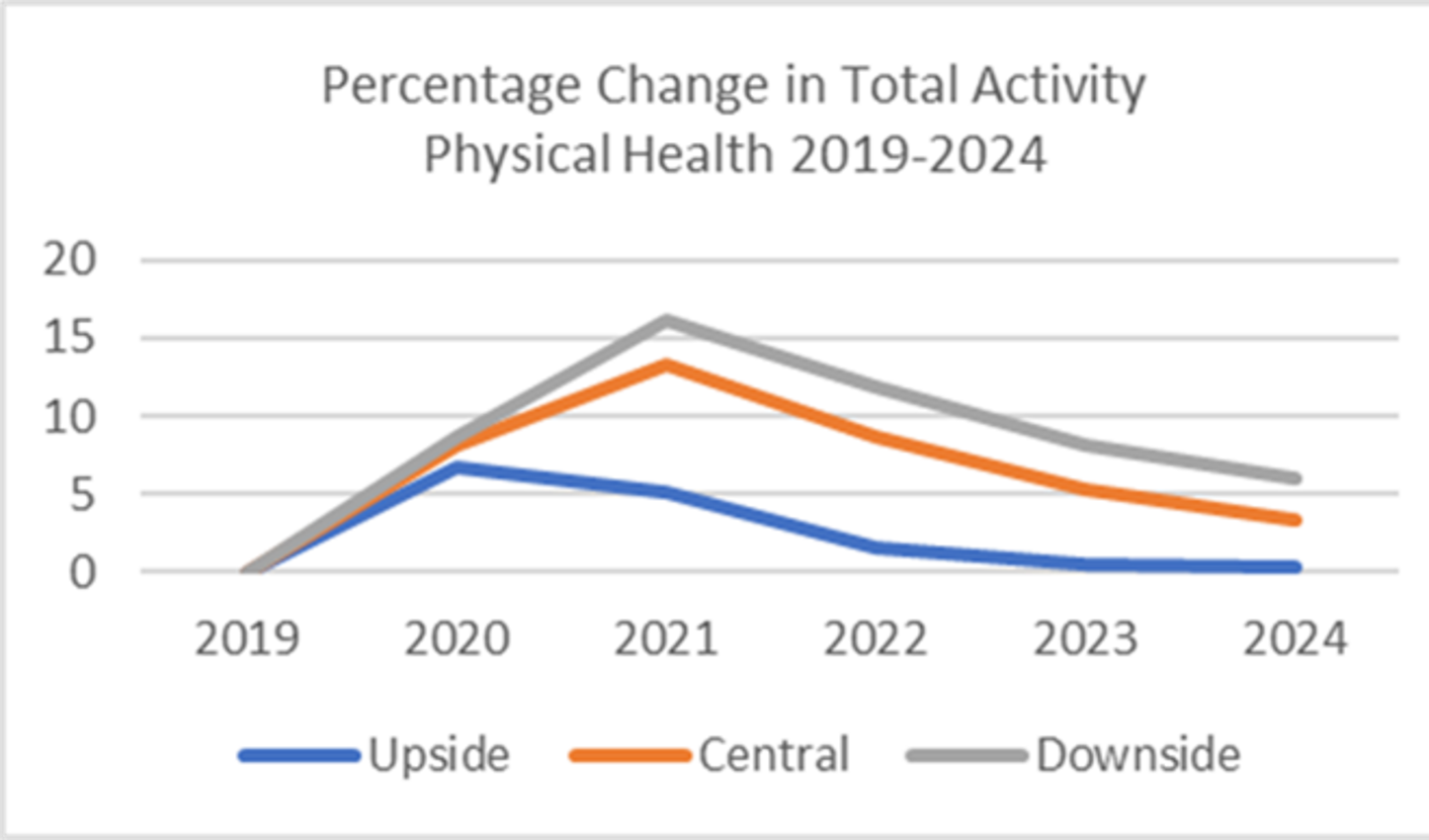
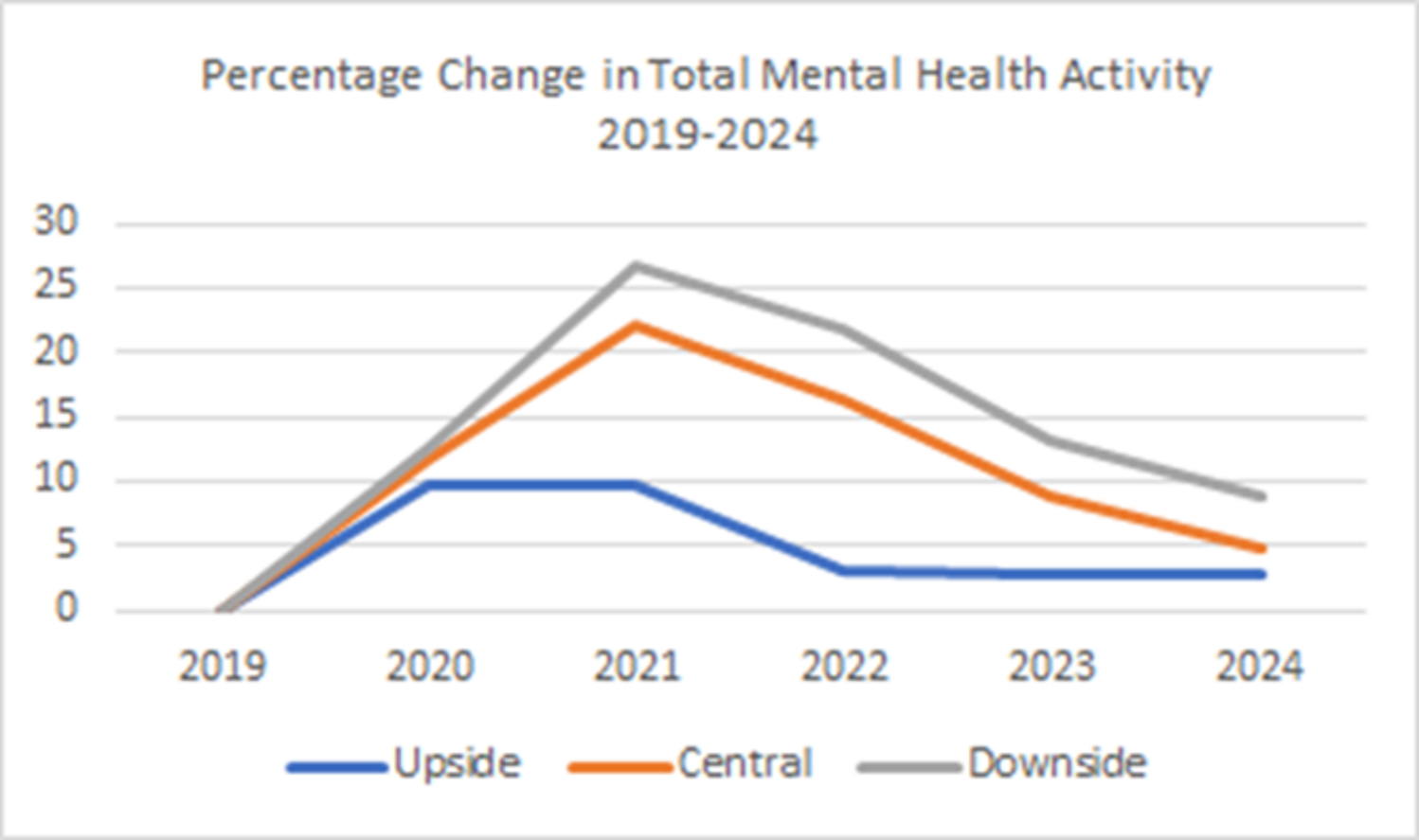
Modelling undertaken by the Strategy Unit, based on the Office for Budget Responsibility’s economic scenarios and the Institute for Fiscal Studies research into the links between employment and health, estimates that the socio-economic impacts alone could generate additional demand of up to 16% for physical health services and 27% for mental health services.
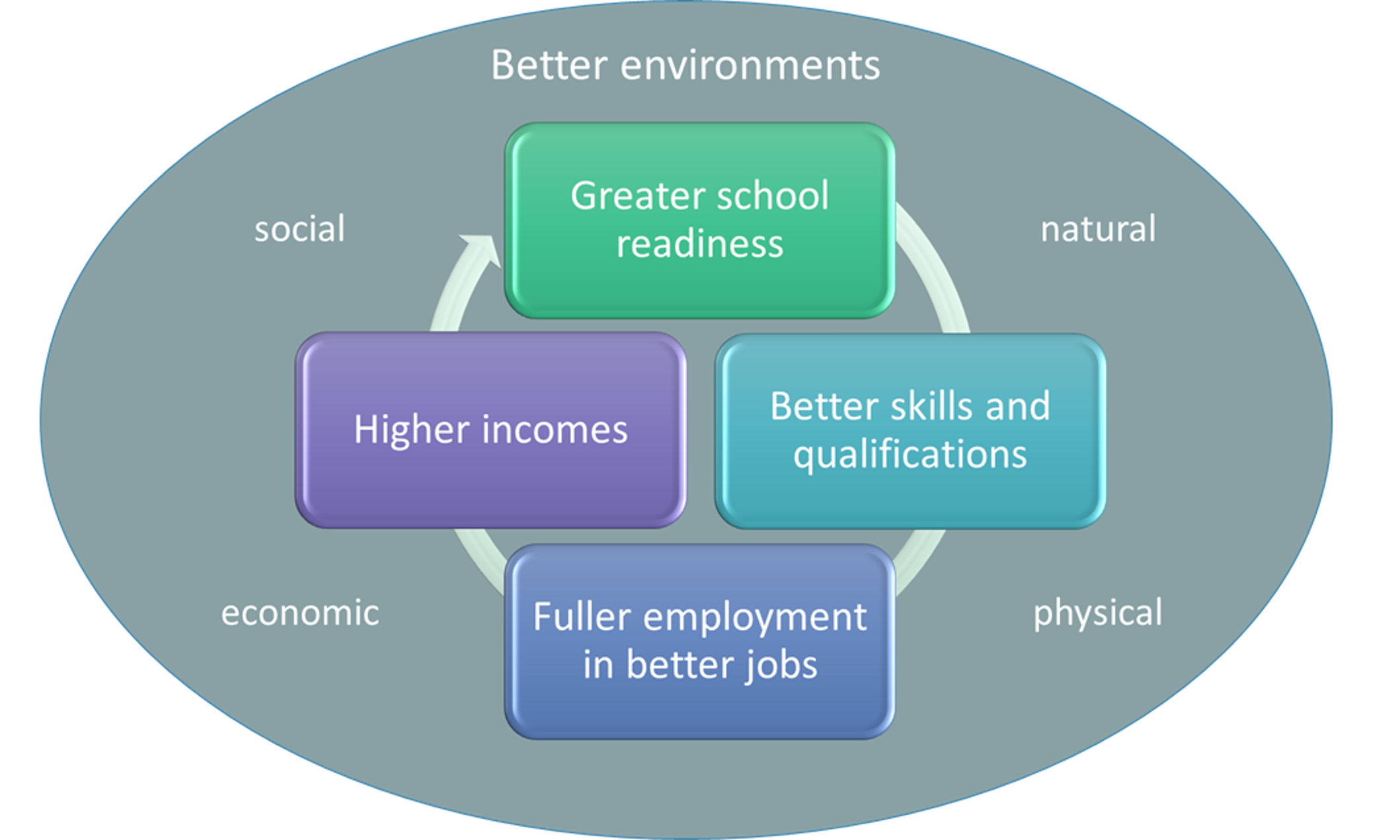
This illustrative modelling has been undertaken as part of our partnership with the Healthier Futures Academy in the Black Country and West Birmingham, and with additional analysis by the Black Country Consortium’s Economic Intelligence Unit. It is intended as the basis for conversations with citizens and partner organisations about how the NHS can be a more effective ‘anchor’ institution in the local economy, to break the cycle of deprivation and ill-health and replace it with a virtuous circle.
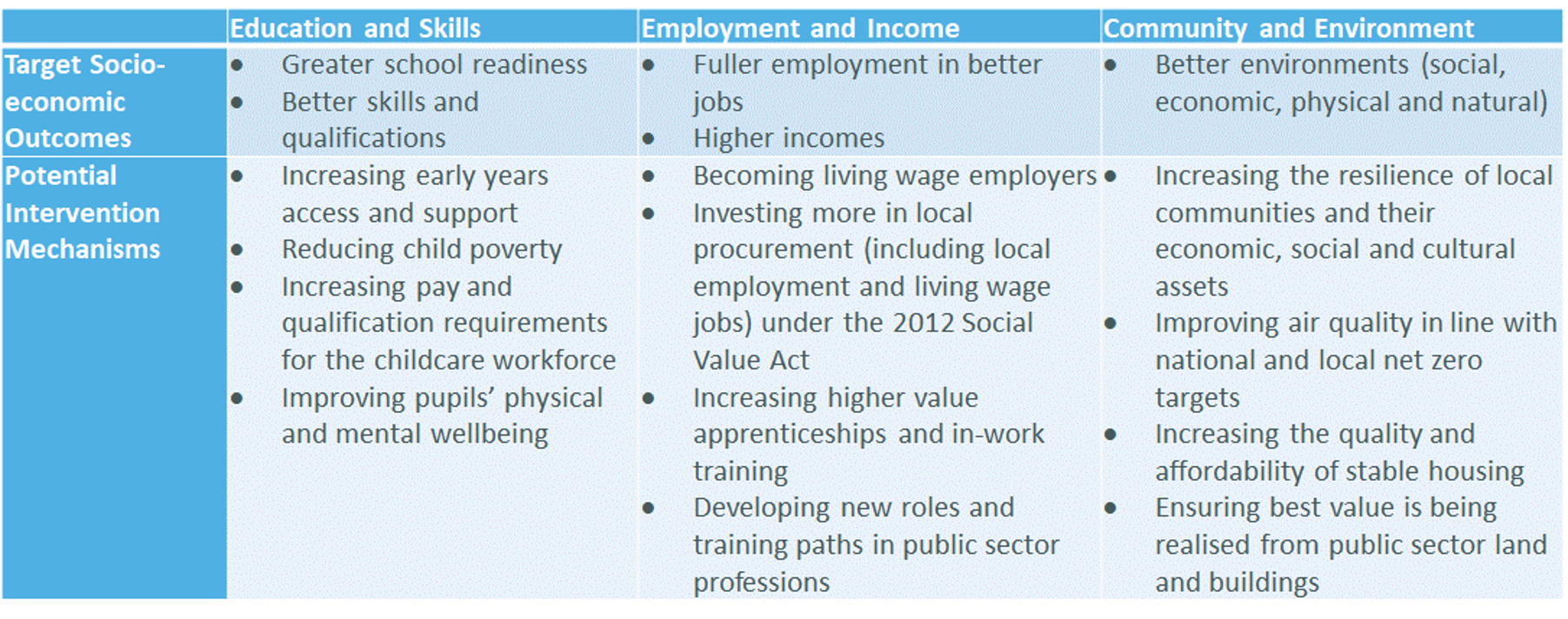
Local partners are being invited to consider with citizens which outcomes to prioritise – where to intervene in the cycle of deprivation and ill-health – and to explore which evidence-based intervention mechanisms may be most appropriate to local needs.
For further information please contact:
In addition to the materials below, physical healthcare and mental healthcare modelling tools are available to health and care organisations in the Black Country and West Birmingham.
CC BY-NC-ND 4.0

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.