To accompany and enrich our analysis of service use in the last two years of life we are producing a set of accompanying blog pieces.
In this blog, the author of ‘The Way We Die Now’ - Seamus O’Mahony – sets our findings into a broader context. He also examines one topic raised in our analysis: chemotherapy at the end of life.
In 2008, the National Confidential Enquiry into Patient Outcome and Death (NCEPOD) published its report “Systemic anti-cancer therapy: For better, for worse? This was a review of the care of over 1,000 patients who died within 30 days of receiving chemotherapy.
Prof Tom Treasure, the chairman of NCEPOD, wrote: “The topics chosen for study by NCEPOD arise from concerns expressed by health professionals and the public . . . Chemotherapy near the end of life is a prime example.” The reviewers judged that care was good in just over one third, that chemotherapy had caused or hastened death in 27 per cent, and that too many patients with poor performance status (grade 3 or 4) were being given palliative chemotherapy.
The report recommended that all deaths within 30 days of chemotherapy should be considered at a morbidity and mortality meeting. This metric is often suggested as a surrogate marker for poor care.
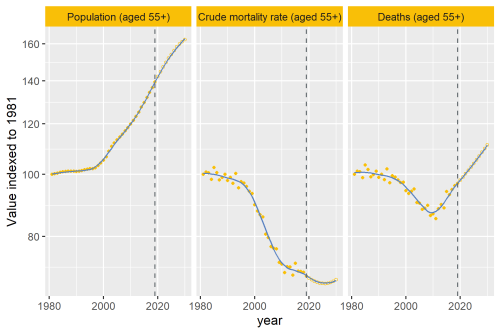
Twelve years on, the Strategy Unit’s report, “End of life care: Healthcare use in the last two years of life”, makes similarly grim reading. Sixteen per cent of patients in this report received chemotherapy in the last four weeks of life: a quarter of these started chemotherapy during their last month. They tended to be younger, and were more likely to have head & neck, pancreatic or haematological cancers.
End-of-life palliative chemotherapy does not improve quality of life and is associated with greater costs and more side-effects. In 2012, the American Society of Clinical Oncology (ASCO) identified the elimination of this practice as the first of its five key opportunities to improve care and reduce costs: “Do not use cancer-directed therapy for patients with solid tumors who have the following characteristics: low performance status (3 0r 4), no benefit from prior evidence-based interventions, not eligible for a clinical trial, and with no strong evidence supporting the clinical value of further anticancer treatment.” Despite this declaration, a recent US study (published in the Journal of Clinical Oncology) reported that 19.6% of 2,858 patients with solid tumours received chemotherapy in the last 2 weeks of life.
Why, then, does this practice continue? Many patients with advanced cancer believe that chemotherapy will cure them, and oncologists are sometimes reluctant to disabuse them of this belief. Patients understandably wish to maintain hope and exercise some degree of control. Some oncologists avoid the “difficult conversation”, fearing the emotional distress it may cause for both patient and doctor. Palliative care services often only become involved after a sudden catastrophe in the days or weeks before death.
How do we change this? NCEPOD’s 2008 report and ASCO’s 2012 declaration have had little effect. Medical care in countries such as the UK has become increasingly splintered, with poor communication and co-ordination between specialities, between hospitals and community services.
One potential approach to the problem of end-of-life chemotherapy might be to involve palliative care physicians and GPs in cancer MDT meetings, as already happens in some countries. More importantly – and more difficult – is the acceptance that the “difficult conversation” should become the essential conversation: this conversation should be the responsibility of the doctor and the right of the patient.