In 2023/24, one million people who were admitted to an NHS hospital in an emergency, were later discharged without a diagnosis. This long-read examines what this means for patients and providers.
Executive summary
|
Diagnosis plays a central role in the medical process, so what does it mean when a patient is admitted to hospital in an emergency but is later discharged without a diagnosis? In this analysis, funded by the Health Foundation, we explore the circumstances that lead to this outcome, and consider whether these cases signal opportunities to improve patient care or hospital efficiency. We found that:
We describe each of these classes and discuss how service improvement efforts can be tailored to each. Further work to determine the relative size of these classes and to test the validity of the classification, is warranted. |
Introduction
Each week, more than 100 thousand people in England are admitted to hospital in an emergency. In most cases, by the time a patient is discharged, the clinical team has reached a view about the underlying medical condition that led to their admission. However, for a sizeable minority of patients, this is not the case: their medical records describe the signs and symptoms that the medical team observed, but not a specific diagnosis.
Although large, the “signs and symptoms” group receives comparatively little attention by researchers, precisely because the absence of a diagnosis means that these patients are difficult to characterise. But anonymised administrative datasets are rich in detail, and if examined carefully, can provide clues that might help us understand whether these admissions were warranted; whether they could have been prevented; and whether opportunities to reach a diagnosis were missed. At a time when hospitals are experiencing significant pressure, this information would seem to be highly valuable.
In this article, we take a closer look at patients who are admitted in an emergency in England in 2023/24, who were later discharged without a diagnosis. For detailed information about the datasets and the methods we used, please see the attached working paper.
Emergency admission: the end of an escalation process
When a patient is admitted to hospital in an emergency, it represents a serious medical incident. Patients with readily treatable or less urgent conditions are usually managed in other parts of the healthcare system, such as primary care, ambulance services, and emergency departments. Admission to hospital can therefore be seen as the end of a medical escalation process, which selects those patients whose immediate needs cannot be safely handled elsewhere.
In 2023/24, there were 6.5 million emergency hospital admissions in England, and most hospital beds were occupied by patients admitted in this way. Emergency hospital admissions are more common in the very young, and the very old, and occur more frequently - at any given age - amongst people living in the most deprived parts of the country. About a third of patients who are admitted in an emergency will be discharged the same day. Most stay for a few days, whilst a small number remain in hospital for an extended period.
One in every six patients
Information about emergency hospital admissions in England is collated within the Hospital Episodes Statistics for Admitted Patient Care data product. Within this dataset, each record represents a period of care (an episode) where an admitted patient was treated by a doctor within a particular medical or surgical specialty. A hospital stay may comprise of one or more episodes. The record for each episode contains a range of administrative, demographic, and clinical information about the patient, including the primary diagnosis - the condition that gave rise to their admission. This is recorded using version 10 of the International Classification of Diseases (ICD-10). The classification system contains more than 14,000 distinct codes, in 22 chapters. A code commonly represents a specific diagnosis, but the classification system also includes codes for symptoms; external causes of morbidity; and factors influencing health status and contact with health services. When a patient’s stay in hospital includes more than one episode, the primary diagnosis can be updated from episode to episode to reflect the latest view of the medical team.
The eighteenth chapter of ICD10, (sometimes referred to as chapter R, since this is the first character of the relevant ICD-10 codes) is somewhat unusual. Unlike those in other chapters, these codes do not represent specific diseases, but rather “signs, symptoms and abnormal clinical and laboratory findings not elsewhere classified”. Codes in this chapter represent, for example, abdominal pain, headache, syncope, confusion, and unsteadiness. Researchers increasingly refer to patients who are assigned an R chapter code as having a ‘non-specific diagnosis’.
Our analysis suggests that 17%, or roughly 1 in 6 patients admitted in an emergency in England in 2023/24 were later discharged with a non-specific diagnosis. This represents 1.08 million hospital spells.
Why diagnosis matters
Diagnosis, the process of determining and assigning a specific disease to a presenting patient, is a central pillar of medical practice. It informs prognosis and guides treatment decisions. The process commonly relies on several sources of information: signs and symptoms identified by physical examination; history obtained by medical interviews; and medical tests.
Meier (2024), points out that leaving hospital without a diagnosis creates uncertainties for those responsible for treating and caring for the patient after discharge. Wen (2015) and Arvig (2022) suggest that patients, too, may benefit from receiving a specific pathophysiologic diagnosis, which may reduce anxiety levels and unscheduled returns to hospital. Hart (2021) discusses the extent to which clinicians should communicate diagnostic uncertainties to the patient, the potential consequences of this decision, and how this interacts with the patient’s own working diagnoses.
Two very different concerns
A small number of earlier studies have considered this group of patients who are discharged without a diagnosis following a non-elective inpatient stay. A further set of papers consider an aligned group of patients: those who are discharged from an emergency department without a diagnosis. Whilst not directly considered in this analysis, papers about the experience of this aligned patient group also provide some useful insight.
These papers appear to be exercised by two quite distinct concerns. Some researchers seem to be worried that the failure to assign a diagnosis might represent a missed opportunity to initiate treatment and prevent harm. These papers often examine the re-attendance, readmission, or mortality rates of these patients to test their theories.
Other researchers are troubled by a very different issue: whether these patients should have been admitted to hospital (or attended ED) in the first place. They seem particularly concerned that these patients might be adding to the pressure that hospitals are facing, and test their theories by identifying patterns in patients’ prior healthcare use (e.g. to flag patients as ‘frequent flyers’).
What have earlier studies found?
The cohort of interest in this study - patients who are discharged following an unplanned hospital stay without a specific diagnosis - is somewhat challenging to isolate in the literature. The terms, “non-specific condition” (NSC) and “non-specific diagnosis” (NSD) are commonly used. Kemp (2020) points out that NSC is a comparatively new concept and therefore “its definition has not yet been formally established”. Many researchers use some or all of the conditions captured in Chapter XVIII of ICD-10 (Symptoms, Signs, and Abnormal Clinical and Laboratory Findings, Not Elsewhere Classified) to define this group. The conditions in Chapter XVIII are sometimes referred to as R-code conditions, since this is the first character of the relevant ICD-10 code. Some studies also include some or all of the codes within Chapter XXI (Factors Influencing Health Status and Contact with Health Services), Z codes. Others still, identify the cohort by excluding various more specific diagnoses. Our summary of the literature for each topic runs in chronological order, to illustrate how the research has developed.
Although earlier studies had touched on the topic, a 2007 review by a UK researcher, Professor Bronagh Walsh, appears to be the first to specifically address the epidemiology of hospital inpatients with ill-defined conditions. The review was focused on older adults who were admitted without a specific diagnosis. At this stage, Walsh concludes that there was no evidence that these admissions were either inappropriate or psycho-social in origin. In 2011, the same researcher published an empirical study, a single-site, retrospective analysis of unplanned admissions of older people, finding that 21.6% of these patients were discharged with R codes. Furthermore, compared to patients who received a specific diagnosis, these patients were more likely to have been admitted via ED (rather than via GP) and out of hours. Their hospital stays were shorter, with fewer inter-hospital transfers, and were less likely to end in death. Walsh found that although these patients were less likely to be readmitted in general, they were more likely to be readmitted with an R-code condition. A more recent multi-region Danish study by Gregerson (2024) found that, having controlled for confounders, the mean mortality rate for patients with and without a specific diagnosis was similar.
Whilst these were the only studies that considered all forms of NSD discharges that we were able to identify, other researchers have explored patients discharged with particular NSD presentations. Ravn-Christensen (2019) found that 6% of patients discharged with an abdominal pain NSD, were readmitted within 3 months and diagnosed with a specific digestive-system disorder. A US study by Martsolf (2020) found that 8.6% of patients discharged from an inpatient setting with a non-specific chest pain diagnosis, returned to hospital (most commonly ED), within 7 days, although rarely with acute coronary symptoms. Exarchakou (2024) examined the hospital use of a subset of UK patients two years before they were diagnosed with colon cancer. Prior unplanned hospital stays with an abdominal pain NSD at discharge were not uncommon, and were more frequent amongst those living in the most deprived areas.
Other researchers have explored the characteristics and outcomes of an aligned patient group: those who received a non-specific diagnosis in an ED. A single site study in Switzerland by Nemec (2010) found that 13.5% of non-trauma ED patients left with a non-specific diagnosis. Almost 7 in 10 of these patients were women, 46% were admitted to a hospital bed from the ED, and 59% had been diagnosed with a serious condition on 30-day follow-up. Mortality at 30 days was 6%. Wachelder (2017 and 2019) found that patients with a non-specific condition at a single ED in the Netherlands were more likely to have been referred by GP, more likely to be admitted, and had higher mortality rates than patients who received a specific diagnosis. Sauter (2018) studied the ED attendances and subsequent admissions of patients with specific and non-specific conditions attending a single hospital in Switzerland. NSC patients had more previous medical contacts, had longer stays in hospital, and had higher mortality rates. Nielsen (2020) conducted a cohort study of patients conveyed by ambulance to EDs in a region of Denmark, who received a non-specific diagnosis. The 30-day mortality rate of his cohort was 6%. A review by Kemp (2020) found that this outcome was more common in older adults. Many of these patients were admitted, and in-hospital mortality was high. A single-site study in Ireland by Conway (2021) concluded that non-specific diagnosis in ED was not prognostic and did not predict in-hospital length of stay or resource use. Birrenbach (2021) found that patients who received a non-specific diagnosis in a single ED in Switzerland received lower rates of diagnostic testing and consumed lower resources than patients who received a specific diagnosis. A 2022 study by the same author found that most patients who received a non-specific diagnosis in ED and who were subsequently admitted, also left hospital without a specific diagnosis. Arvig (2022) examined a single ED in Denmark and found that mortality at 30 days was associated with a non-specific diagnosis. A systematic review by Orlando (2023) found that the risk of hospitalisation for non-specific lower back pain was associated with pain distress, residing alone, ethnicity, compensable status, younger workers, residential and hospital contextual factors, emergency department triage category, hospital specialty classification, and utilisation of emergency department investigational resources.
Two researchers explored trends in the occurrence of discharge from ED without a specific diagnosis. Wen (2015) found that in the US, between 1993 and 2009, the incidence of patients leaving ED without a pathological diagnosis had increased. Kenner (2019) reached a similar conclusion for an Australian cohort between 2000 and 2018.
The researchers exploring this phenomenon offered several potential reasons why patients leave ED without a diagnosis. These included (1) that no pathology was present; (2) that symptoms resolved during the ED stay; (3) that tests and investigations were required that could not be carried out in ED; (4) concern that misdiagnosis might lead to malpractice claims; (5) the impact of diagnosis on patient charges; and (6) ED crowding and clinician busyness.
A further set of papers, relating to both inpatient and ED care, describe systematic demographic and socio-economic bias in diagnosis. Bell (2023) found that a high proportion of US patients who experienced diagnostic errors had limited English-language health literacy or experienced socio-economic deprivation. National Voices (2024) also identified a lack of access to language interpretation as a barrier to diagnosis in England. A systematic review by Herasevich (2023) found that some ethnic groups experienced higher odds of a diagnostic error for acute myocardial infarction and acute coronary syndrome. Jones (2022) found that Māori patients attending an ED in New Zealand were more likely to leave without a confirmed diagnosis, however, the authors concluded that this was due to a failure to extract the diagnosis from electronic records. A cross-sectional study by Ellenbogen (2024) of patients discharged from EDs in several US states, found that Black patients who were discharged without a specific diagnosis, received fewer diagnostic tests than their White counterparts. Samms (2025) reports a five-fold variation in ME/CFS diagnosis by ethnicity and states that this scale of variation cannot be readily explained by differences in genetics or access to primary care. A multi-centre cohort study in Spain by Sempere (2023) found that women experience greater delays in diagnosis for irritable bowel syndrome than men. Finally, an Australian cohort study by Dawson (2022) found that socioeconomically disadvantaged patients who attend ED with non-specific chest pain might be inappropriately discharged in some circumstances.
The search strategy employed in this scoping review can be found here
Who are these patients and what are their symptoms?
In Table 1, we present information about the age and sex of patients who received non-specific primary diagnoses in the discharge episode, the NSD group, and those who received other diagnoses, the reference group. The data relate to patients living in England who admitted to hospital in an emergency during 2023/24.
Table 1: Age and sex of patients discharged with a non-specific diagnosis, England, 2023-24
|
Non-specific diagnosis (NSD): Spells (%) |
Specific diagnosis (SD): Spells (%) |
Difference in % |
||
|---|---|---|---|---|
|
Total |
- |
1,076,089 (100%) |
5,238,803 (100%) |
0.0% |
|
Sex |
Female |
601,656 (55.9%) |
2,735,485 (52.2%) |
3.7% |
|
Male |
474,433 (44.1%) |
2,503,318 (47.8%) |
−3.7% |
|
|
Age group |
0-10 |
108,816 (10.1%) |
612,930 (11.7%) |
−1.6% |
|
11-17 |
20,819 (1.9%) |
70,827 (1.4%) |
0.6% |
|
|
18-64 |
566,049 (52.6%) |
2,200,165 (42.0%) |
10.6% |
|
|
65+ |
380,405 (35.4%) |
2,354,881 (45.0%) |
−9.6% |
Approximately 56% of those discharged with an NSD were female, compared to 52% of those in the reference group. Having been admitted, women are more likely than men to be discharged without a diagnosis (18% vs. 16%). Having controlled for differences in population age-structure, women are 48% more likely to experience a hospital spell that concluded without a specific diagnosis.
Women of Pakistani and Bangladeshi ethnicity, and to a lesser extent men, were more likely than their White counterparts to experience a hospital spell that concluded without a specific diagnosis.1 This is true having adjusted for differences in the age structure of these populations. We note that in the 2011 Census, 11.1% of people aged over 3 year of Pakistani ethnicity and 16.2% of those of Bangladeshi ethnicity, reported that they could not speak English or Welsh well, higher than most other ethnicities. In these groups, rates were higher amongst for women and for those aged over 45 years. This may be relevant given the centrality of patient-clinician communication to the diagnosis process.
Although people living in more deprived areas are more likely to be admitted to hospital in an emergency, having been admitted, they were no more likely to be discharged without a diagnosis.
In terms of age, over half of NSD spells involved patients aged between 18 and 64 years. The probability of being discharged without a diagnosis was higher in the 11-17 and 18-64 age groups than in older or younger groups.
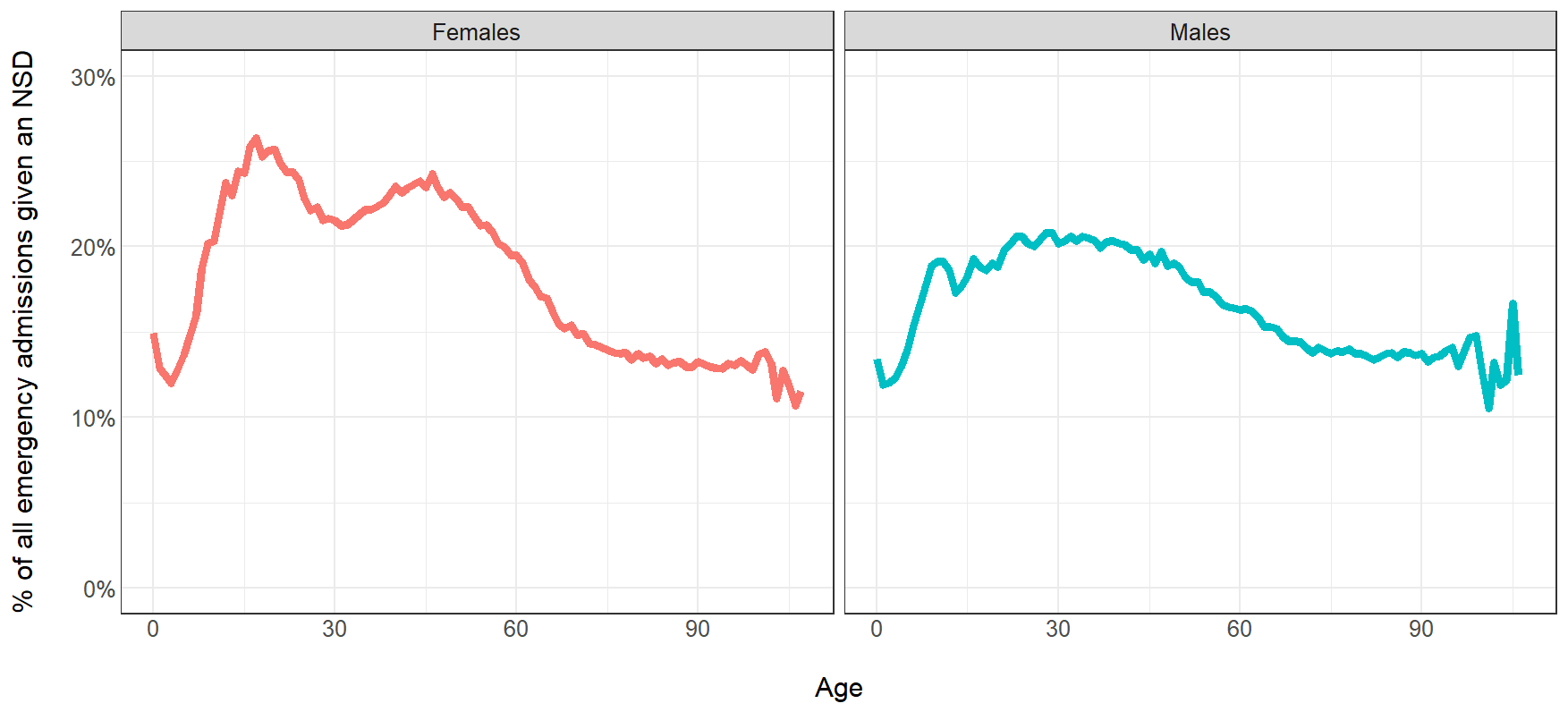
The chance of being discharged without a diagnosis was most pronounced amongst female inpatients in two age segments: 14 to 23 years and 40 to 50 years (see figure 1).
1Variations were seen in other ethnic categories, but these categories were small in size and less well defined, making it difficult to interpret the results.
Figure 1: NSD spells as a percentage of all spells, by age and sex, England, 2023-24
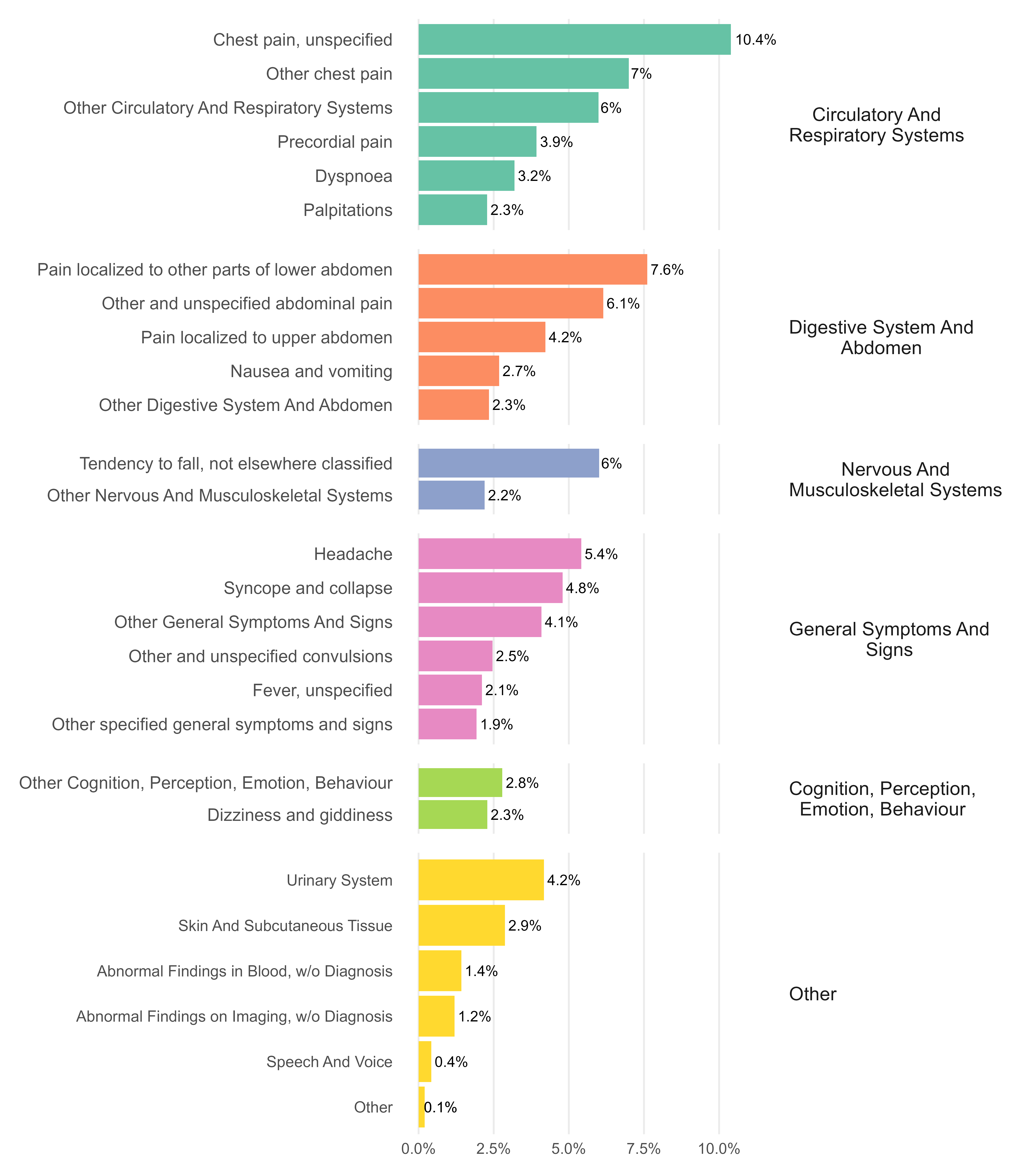
Figure 2 shows the frequency of primary, non-specific diagnoses in 2023/24. Symptoms relating to the circulatory and respiratory system were most common, followed by those relating to the digestive system and abdomen. Taken together, these account for more than half of all NSD spells. Tendency to fall, headache, syncope, convulsions, fever, and dizziness were also common.
Figure 2: Non-specific diagnoses as % of all NSD spells, England, 2023-24
The age and sex profiles of NSD spells for each of these signs and symptoms are quite distinct. As one might expect, NSD spells for fever and convulsions are almost exclusively associated with young children, and tendency to fall occurs mainly in those aged over 75 years. Abdominal pain is higher among younger females, while chest pain diagnoses are highest in middle age for both sexes. There is a very specific peak in signs and symptoms involving emotional state amongst women aged 14-18 years. For males aged 18 – 64, chest pain is the most common NSD. NSD spells with headache and syncope are widely distributed by age and sex.
For the remainder of this analysis, we focus on the experience of patients aged 11-64 years, since discharge without diagnosis following an emergency admission is particularly common in this cohort.
Most patients are admitted via the emergency departments, but patients who are admitted on the advice of their GP are more likely to be discharged without a specific diagnosis. Most NSD patients are admitted during the day, on a weekday. Patients admitted out of hours and on weekends are less likely to be discharged without a diagnosis.
For some of these spells there are indications that the medical team reached a quick conclusion that no further action was warranted. Roughly one in three received no intervention or procedure and a similar proportion received no diagnostic test2. Seven in ten were discharged without an overnight stay. Almost nine in ten had no or only limited comorbidities. Where comorbidities were noted, hypertension was common in both sexes, but more often in men. Asthma was also fairly common. Anxiety, and depressive symptoms were sometimes noted in women, and a history of psychoactive substance misuse use in men.
More than half of NSD patients are managed by consultants in the emergency medicine and general internal medicine specialties. One in six female NSD patients and one in nine male NSD patients are managed by the general surgery specialty.
A small, but not insignificant proportion (c. 2-3%) of NSD patients self-discharge, perhaps limiting the opportunity for clinicians to determine a specific diagnosis.
2 We counted tests described in the guidance for the DM01 return. https://digital.nhs.uk/binaries/content/assets/website-assets/data-and-information/data-collections/diagnostic-waiting-times/dm01-guidance-v8.pdf
Looking forwards and looking back
By linking patients’ medical records over time, it is possible to incorporate knowledge about prior or subsequent hospital activity, and build a richer picture of the experiences of these patients.
About one fifth of NSD patients had been admitted to hospital in the 90 days before their NSD spell. This is not unusual. Hospital activity commonly exhibits high levels of temporal clustering. Indeed, the figure is slightly higher amongst patients who were discharged with a specific diagnosis.
Close to a third of NSD patients were admitted again in the 90 days after discharge. This experience was slightly more common amongst women than men. When readmission did occur, many (about one third) were again discharged without a specific diagnosis. Where a specific diagnosis was given in subsequent spells, these tended to be digestive, circulatory, and respiratory system disorders.
Around 40% of NSD patients were referred for an outpatient consultation in the 30 days after leaving hospital. Referral rates were slightly lower than for patients who were discharged with a specific diagnosis. Referral to cardiology, clinical physiology, and neurology were more common amongst NSD patients. Less than 3% of female NSD patients were referred for a gynaecology outpatient appointment: two thirds of the rate at which other female inpatients were referred.
Further details of the data sources, definitions and methods used in this analysis can be found here
Insights from clinicians
Although the data and prior research are rich in detail, they are nonetheless abstractions or representations of the reality of care delivered by clinicians and experienced by patients. To ground our analysis, we conducted semi-structured interviews with five clinicians working with patients admitted in an emergency. During the interviews, we asked clinicians about their reflections on the headline results from our analysis, and their perspective on why patients are frequently discharged without a specific diagnosis. We provide a summary of these discussions below, but a more detailed description of this qualitative research, the methods and findings, can be found here.
In many ways, the clinicians reported that our analysis matched with their experience. They were unsurprised with our findings relating to the proportion of patients who were discharged without a diagnosis, and with the over-representation of women and certain ethnic groups.
The clinicians described several circumstances or mechanisms that lead to patients being admitted and then discharged without a diagnosis. They described the need to manage risk and provide a place of safety to people presenting with psychosocial, emotional, and psychiatric distress. In some cases, patients were admitted for further tests, when discerning the seriousness of a presenting condition in a busy emergency department was challenging. Clinicians spoke here about acute and recurrent chest pain, abdominal pain and vomiting, and gynaecological pain.
Several potential explanations for the over-representation of women in the NSD cohort were offered, including medical misogyny leading to the normalisation of female pain, higher levels of health seeking behaviour amongst women, and the absence of clear pathways for some sex-specific conditions affecting women. Whilst clinicians were not surprised with the high rates of NSD spells amongst younger female patients that were observed in the data, they were not necessarily expecting the second peak in NSD spells amongst women aged 45-60. They speculated that this second peak might indicate dismissal of menopause-related health issues.
The clinicians found it more difficult to explain why there would be an over-representation of certain ethnicities in the NSD cohort. Nonetheless some theories were put forward. These included language barriers, cultural disconnects between the patient and clinician, excessive deference to medical professionals, and institutional biases influencing the quality of the diagnosis process. Clinicians also discussed whether discharge thresholds may be lower amongst certain ethnic groups where the clinician had determined or assumed that familial support could be relied upon after discharge.
There was a broad acknowledgement that being discharged without a diagnosis could have negative consequences: for the patient, their carers, and for clinicians who work with the patient in the community. But there was also a recognition that endlessly seeking ever-more precise diagnoses risked over-medicalisation, and could draw resources from other patients and services with a greater capacity to benefit. Indeed, in some circumstances, the interviewees saw discharging a patient without a diagnosis as a necessary or even optimal outcome, that required experienced and confident clinicians.
Four patient classes
This descriptive analysis, which looks at patients who leave hospital after an unplanned admission without a specific diagnosis, cannot easily be resolved into a single unifying narrative. Such a tension is also seen in the published literature on the topic: Do these admissions indicate systemic failures in hospital processes, or systematic bias in medical treatment? Are these unnecessary admissions arising from trivial or non-medical conditions? Or perhaps we should view these events as a necessary step in a clinical process that requires more time and information before a diagnosis can be assigned? One way to reconcile these apparently contradictory perspectives is to regard the cohort as being made up of a set of often quite distinct patient classes. Identifying these classes may help unlock the debate and lead to a range of more specific investigations and service improvement initiatives.
We set out below, a potential set of patient class descriptions, informed by the descriptive analysis and the scoping review of the literature. These were tested and refined these descriptions through discussions with clinicians described above.
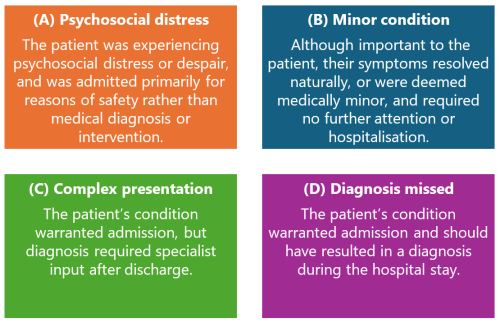
Figure 3: Discharged without a diagnosis – a typology
We describe each class in more detail below, providing suggestions on how these cases might be identified in routine administrative datasets, and how care of these patients might be improved.
Table 2: Discharged without a diagnosis typology – a description of each type
Psychological distress
| Description | The patient was experiencing psychosocial distress or despair, and was admitted primarily for reasons of safety rather than medical diagnosis or intervention. |
| Characteristics in administrative datasets | There may be evidence of drug or alcohol misuse, or self-harm in the current or previous admissions. Subsequent admissions may occur with a primary diagnosis in ICD-10 Chapter F (Mental and Behavioural Disorders), or codes X60-84 (intentional self-harm), or Y10-34 (an event of undetermined intent) |
| Improvement opportunities | Admission to hospital may have been necessary in the moment but an urgent out-of-hospital intervention may have been preferable. Increasing the capacity out-of-hospital mental health services, may therefore be benefical. Efforts to tackle the underlying social and economic determinants are also warranted. |
Minor Condition
| Description | Although important to the patient, their symptoms resolved naturally or were deemed medically minor, and required no further attention or hospitalisation |
| Characteristics in administrative datasets | These patients are more likely to have been admitted at the instruction of a GP; a generally discharged from hospital on the same day as admission; receive no intervention or diagnostic test in hospital; and have low levels of comorbidities. These admissions may be more common when the patient's stay in ED is approaching 4 hours and when pressure to avoid 4-hour breaches is high. The patients concerned are rarely admitted in the 3 months before, or the 30 days after, admission, and tend not to be referred for an outpatient attendance. |
| Improvement opportunities | What is clear in hindsight may not have been so when the decision to admit was taken. In some cases, the patient's condition may have rapidly improved after admissions. Nonetheless, inasmuch as these admissions could have been avoided, efforts might usefully focus on providing rapid advice to GPs; tracking admission thresholds through EDs and identifying and supporting ED clinicians that appear to admit at lower thresholds than their peers. |
Complex presentation
| Description | The patient's condition warranted admission, but diagnosis required specialist input after discharge |
| Characteristics in administrative datasets |
After the patient is stabilised and discharged, they may be referred for a specialist consultation in an outpatient setting and/or for diagnostic tests. Such patients may have complex structural, psychiatric, or functional conditions, that can only be diagnosed when symptoms advance or persist, and other possible diagnoses have been ruled out. These conditions may appears as primary diagnoses or as comorbidities in subsequent admissions. |
| Improvement opportunities |
Labelling the patient as a "frequent user of unscheduled services" may bias clinicians decisions and hinder efforts to identify the underlying cause of hospitalisation. Increased capacity and capability in community and primary care services may reduce the numbers of these emergency presentations to hospital. Hospitals may wush to consider lowering the threshold for referral to urology and gynaecology services for women presenting with abdominal pain, where no pathology could be identified during the hospital stay. |
Diagnosis missed
| Description | The patient's condition warranted admission and should have resulted in a diagnosis during the hospital stay |
| Characteristics in administrative datasets |
Pressure on hospital beds may have resulted in the patient being discharged too soon. Patients in this class may self-discharge from the index spell before investigations have been completed and/or against clinical advice. These patients may experience a subsequent emergency admission during which a diagnosis for a specific disease or injury is assigned. |
| Improvement opportunities | There may be some failure in the diagnostic process (e.g. poor dialogue between patients and clinicians, poor access to diagnostic testing or failure to interpret the diagnostic test). Systematic bias in medical processes means that this outcome may be more common in women and for patients from minority ethnic groups. Trusts may wish to assure themselves that adequate interpretation services are avaliable in line with recent guidance from NHS England. |
We invite feedback on the utility and value of this classification to support service improvement initiatives. Further work would be required to clinically validate the classification and to explore ways to assign patients to classes.
Conclusions
In this report we present information from published research, primary analysis of routine datasets, and the experience of clinicians, to gain an insight into the incidence, causes, and consequences of leaving hospital without a diagnosis after an unplanned admission. This phenomenon is common, but not homogeneous. We propose a classification of these patients and seek feedback on its utility. Efforts to improve patient experience and service efficiency will need to be tailored to each patient class.
What next?
Building on the work reported here, we set out below, five potential future projects. These projects would aim to further improve our understanding of the patient cohort, to test and validate the proposed patient classes, and to explore the underlying mechanisms at play.
Whilst a narrative description of patient classes may be a useful start, validating and operationalising the concept will require detailed definitions. The purpose of this project would be to develop a set of decision rules or statistical methods that could be used, retrospectively, to assign patients in the cohort to one or more of the patient classes. This would need to take account of variation between hospitals in coding practices. These approaches would be designed to be implemented using standard administrative datasets. Having applied these rules, the size and characteristics of each patient class could be described.
A casefile audit might be used to test and clinically validate the proposed classification system. Appropriately trained clinicians would review the notes of a selection of patients in the cohort and assign each to one or more of the classes. The clinician assignment and the rules-based assignment would be compared and reported. This might lead to changes in the class descriptions or to the rules used to assign patients.
This project would explore one possible explanation for the observation that women are significantly more likely to be discharged without a diagnosis. If this disparity is driven in part by clinician bias, then we might expect some variation in this effect between patients treated by male and female clinicians. The project would seek to estimate the odds of being discharged without a diagnosis, for each of the 4 combinations of male and female patients and clinicians, having controlled for other pre-diagnosis covariates (e.g. age, comorbidities, day of week, admission via ED vs GP, etc).
This project would examine the impact of English language skills and the availability of interpretation services as an explanation for the observation that people from Pakistani and Bangladeshi ethnic origins are more likely to be discharged without a diagnosis. Whilst data on English language skills are not routinely captured in administrative hospital datasets, other data sources provide information on the proportion of the population with different levels of English language skills, by ethnicity, sex and age. The project would estimate the odds of being discharged without a diagnosis by ethnicity, having controlled for casemix. The models would include interaction terms between ethnicity, sex and age. If the profile of results by sex and age, for the Pakistani and Bangladeshi patients, mirror the reported levels of English language skills in these populations by age and sex, then this would provide some support to the theory that poor access to high quality interpretation services is adversely affecting rates of diagnosis.
A recent House of Commons committee report recommended that the NHS collect data on delays in diagnosis and treatment for benign gynaecological conditions, such as endometriosis, adenomyosis, fibroids, and heavy menstrual bleeding. This project would explore what is possible from existing datasets. Where feasible, the project would highlight geographic and socio-demographic variation in diagnosis rates, waiting times, and use of urgent care services. This analysis will be complemented with qualitative research which will illustrate the consequences and causes of missed and delayed diagnosis. The qualitative research would use maximum variation sampling to incorporate a diversity of voices.
CC BY-NC-ND 4.0

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.