An analysis of the physical health of people who use mental health services: life expectancy, acute service use and the potential for improving quality and using resources more efficiently.
The Strategy Unit, inspired by earlier research published by the Nuffield Trust, has created a ground breaking report for all STPs which investigates in detail the interaction between mental and physical health. The work describes and unpacks the gap between the physical health and life expectancy of those in contact with specialist mental health services and the rest of the population, and examines levels of variation in health care utilisation.
‘Making the Case for Integrating Physical and Mental Health Care’ has been designed to inform greater partnership working within local health economies to drive better health outcomes for patients and improved levels of efficiency. The Black Country STP were the pilot area for this work, and subsequently NHS England commissioned a version of the report for all 44 STPs in England. These STP reports were published via STP leads in May 2017 and have received wide-spread acclaim for their quality, depth and real-world practical relevance. We are particularly enthused by the positive reaction from the clinical community, with lots of examples where our work has helped to catalyse clinically- led service improvement initiatives
The reports give STPs bespoke data and analysis, setting out the scope to improve patient care by better integrating mental and physical health services, in line with the ambition set out in the Five Year Forward View for the NHS. They also model potential benefits and opportunities for financial reinvestment from reduced pressure on acute care and elsewhere.
Director of the Strategy Unit, Peter Spilsbury, said: “This report is important. Using newly linked national data and novel analysis, it can unpack for each STP area one of the biggest yet least spoken about health gaps facing our society - the gap between the physical health and life expectancy of those in contact with mental health services and the rest of the population.”
"Some of the differentials in both health outcomes and health service utilisation are eye opening but we have been able to use these findings (and the summary of the evidence base provided) to begin building a broad coalition of local partners to identify and implement practical changes. I commend it enthusiastically to colleagues as a catalyst for much needed change.”
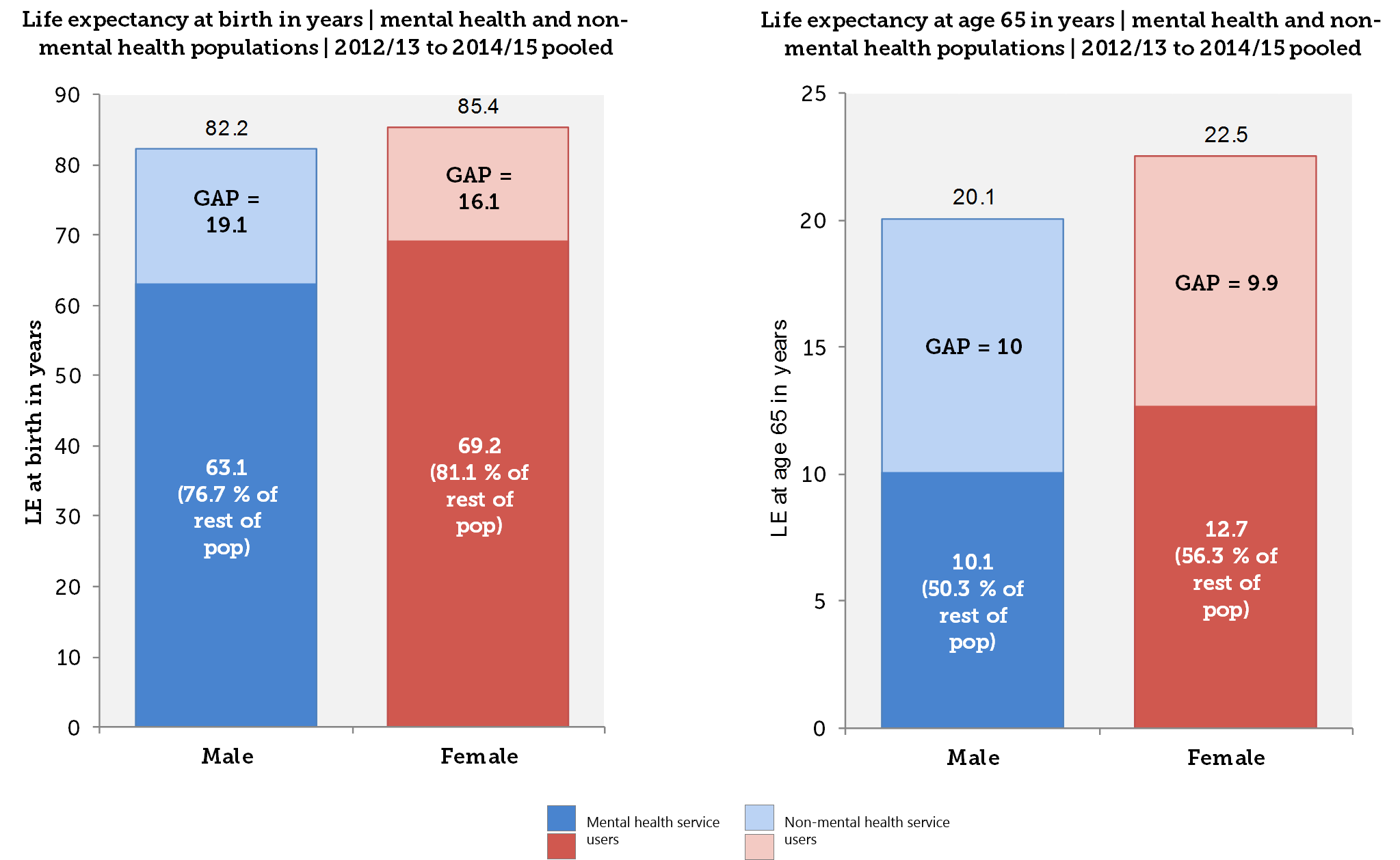
According to the study, men with mental health disorders in England are estimated to live 19 years less than those without. For women this gap is around 16 years and the figures for both can vary substantially between STP localities.
Fig 1. Life expectancies in England for mental health services users and the rest of the population
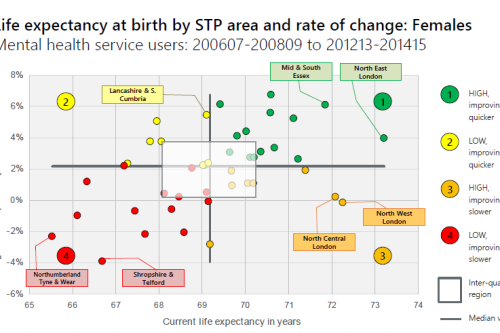
The research, which uses linked national datasets, also reveals that there is a difference of eight years between the lowest and highest mental health life expectancies across STP areas in England.
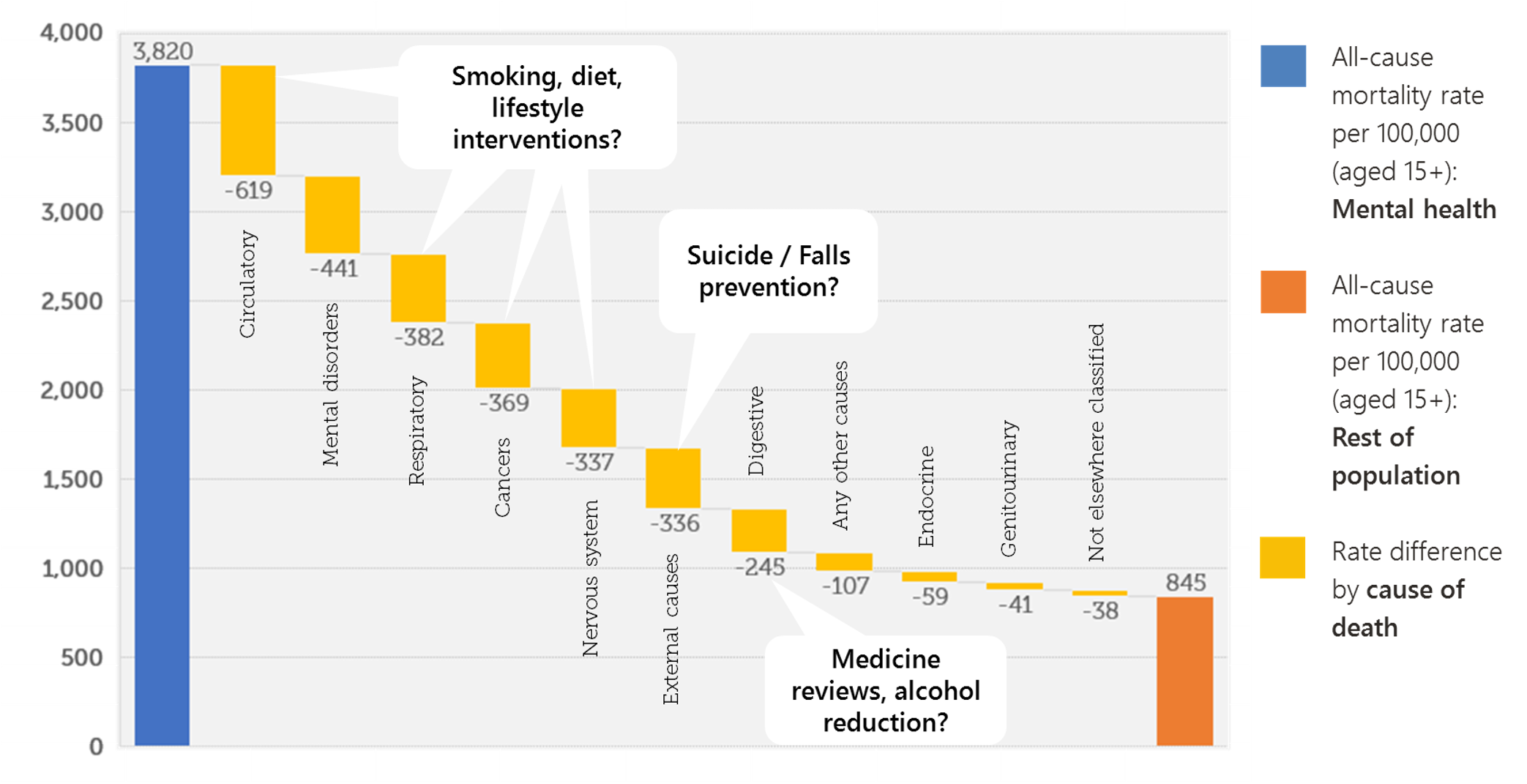
Demographic differences alone cannot explain the range, which suggests that factors related to service provision are significant. Common causes of death for specialist mental health service users do not mirror the rest of the population.
“The headlines from this remarkable report are overwhelming. This report is vitally important and a powerful call to action. For us it has defined a new high priority work stream"
Fig 2. Breaking down the gap in mortality by cause of death (males)
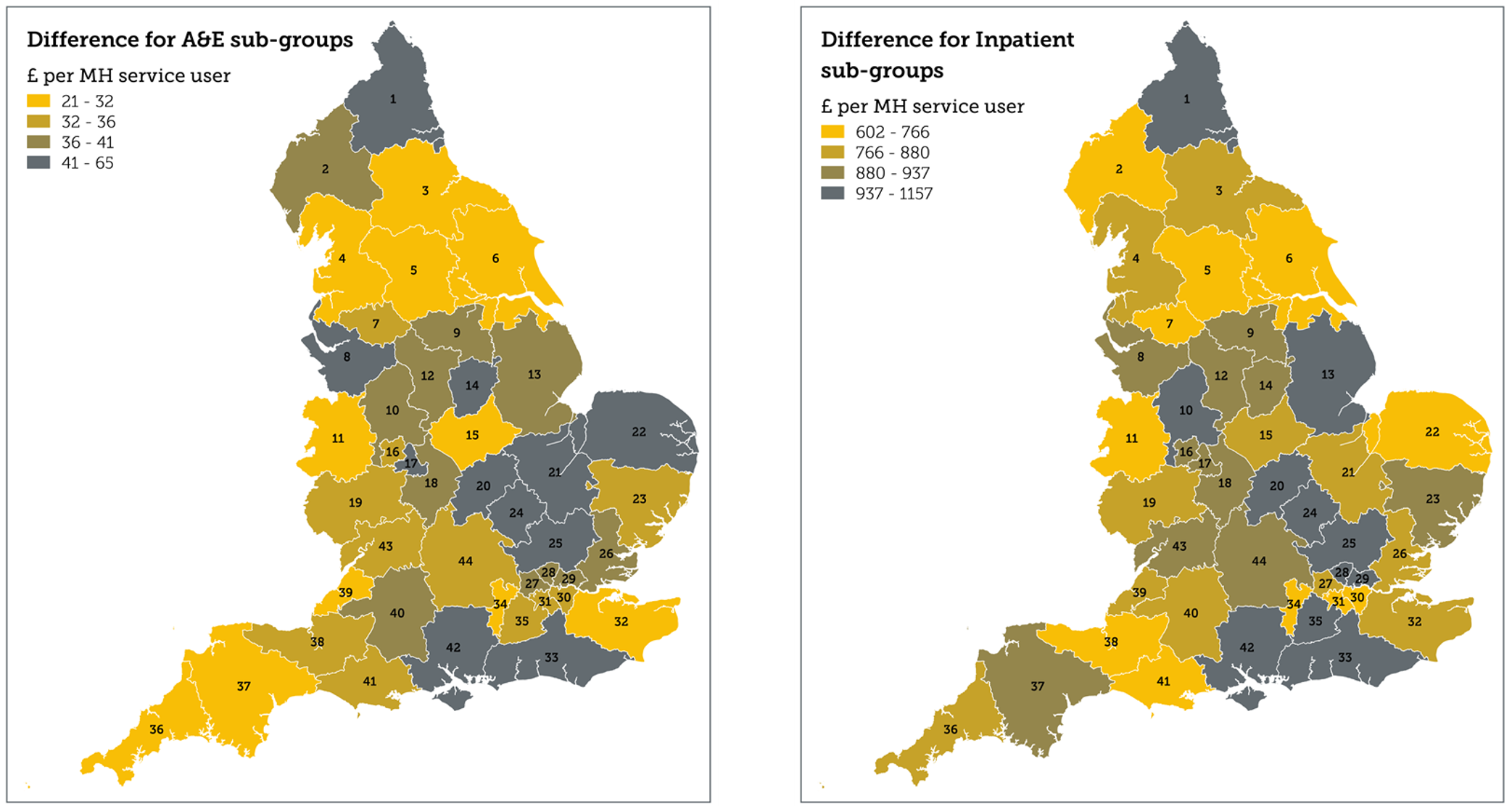
Fig 3. Difference in A&E and inpatient spend per head of service user population by STP area
As this report and analysis makes its journey in the world, we are keen to understand its impact and also to connect with people and initiatives that are responding to the picture it paints. Feedback is really important to us. We ask any interested parties to get in touch so we can build links. As we undertake further work, we will keep on publishing it via this website too.
Making the Case for Integrating Physical and Mental Health Care - STP Area Reports
Please note, these data and reports were produced in 2017 and as such apply to the 44 STP areas at that time.