 Elective care | Emergency care | Policy
Elective care | Emergency care | Policy
How is growth in diagnostic testing affecting the hospital system?
Diagnostic services, such as medical imaging, endoscopy, and pathology, have grown substantially in recent years and at a faster rate than most other healthcare services. Increased diagnostic testing brings benefits to patients, but rapid growth of this service area within a complex, adaptive…
 Better use of analysis | Inequalities
Better use of analysis | Inequalities
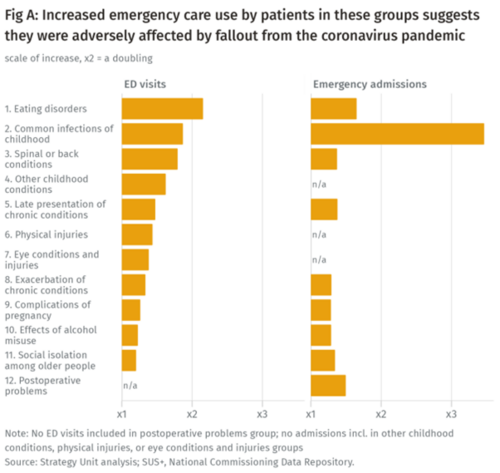
Population health implications of the Covid-19 pandemic
Our new report for The Midlands Decision Support Network (MDSN) presents findings of the effects of the care disruption, from the Covid-19 pandemic, on population health. The in-depth analysis identifies which patients and health conditions should be the focus of future efforts in reducing…
 Elective care | Inequalities | Policy
Elective care | Inequalities | Policy
What are the ethical challenges in addressing inequities?
Produced by Angie Hobbs - the world’s first Professor in the Public Understanding of Philosophy – this paper examines the ethical questions raised by our report outlining strategies for reducing inequity.
 Mental health | Policy
Mental health | Policy
Estimating the impact of the proposed reforms to the Mental Health Act on the workload of psychiatrists
In January 2021, the Government published a White Paper, setting out its plans to reform the Mental Health Act. The Government invited views on the paper and in July 2021, it published a summary of the consultation responses and its plans to address the issues raised. The proposed reforms aim to…
 Mental health | Primary, community and social care services
Mental health | Primary, community and social care services
Inequities in children and young people’s mental health services
Good mental health during early years and childhood has a great bearing on health throughout life. By contrast, poor mental health can cast a long shadow. Consequences may include depression, self-harm, and poor physical health. Services recognise this. They aim to provide access to support in a…
 Inequalities | Policy | Public health and prevention
Inequalities | Policy | Public health and prevention
Measuring the effect of the coronavirus pandemic on population health
Measuring the effect of the coronavirus pandemic on population health One feature of the pandemic has been the fast-flowing stream of facts and numbers about the impact of Covid-19. At the same time, we’ve had to absorb the meaning of terms that were previously the preserve of epidemiologists and…
 Better use of analysis | Elective care | Emergency care | Inequalities | Primary, community and social care services | Public health and prevention
Better use of analysis | Elective care | Emergency care | Inequalities | Primary, community and social care services | Public health and prevention
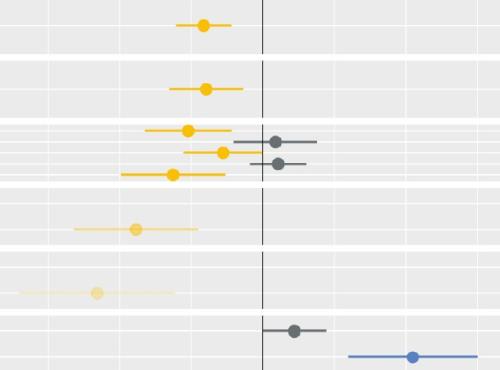
Less noise and more light: using criteria-driven analysis to tackle inequalities
Reducing health inequality is a long-standing aim of health policy. Yet the gap between policy aim and population outcome has grown in recent years: on most measures health inequalities have got worse.
 Elective care | Inequalities | Policy | Primary, community and social care services
Elective care | Inequalities | Policy | Primary, community and social care services
Socio-economic inequalities in access to planned hospital care: causes and consequences
Tacking inequalities in health is a long-standing NHS policy objective. Variation in the experiences and outcomes of different communities during the COVID-19 pandemic served to bring this issue back into focus.
 Inequalities | Policy | Primary, community and social care services | Public health and prevention
Inequalities | Policy | Primary, community and social care services | Public health and prevention
Reviewing the evidence on digital inclusion
Digital technology is a significant part of our daily lives. It has changed the way we interact with each other, the services we use, and the ways we work. The NHS is no exception. Digital technology has begun to change the way health…
 Elective care | Policy | Primary, community and social care services | Public health and prevention
Elective care | Policy | Primary, community and social care services | Public health and prevention
Evidence review: Early diagnosis of cancer
Detecting cancers early is essential to saving lives and reducing the need for invasive treatments. So, in 2019, the NHS Long Term Plan set a national target for increasing the proportion of cancers diagnosed at an early stage. There is room for improvement in current performance. In 2018, 55% of…
 Policy
Policy
A framework for understanding policy change
A new policy, strategic direction or major programme is announced. How do we begin to understand, interpret and explain it? And how can we start the task of analysing and critiquing it? I see three main approaches: 1: Personal views As an individual, we might ask whether we like or agree with the…
 Better use of analysis | Inequalities | Mental health
Better use of analysis | Inequalities | Mental health
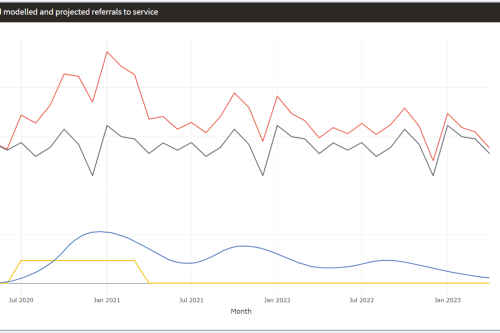
Mental Health Surge Model
Early in the Covid pandemic, it became clear that people’s mental health would suffer. Whether through bereavement, unemployment, social isolation, not being able to access support services – or a host of other routes – an alarming picture began to emerge and attract attention.
 End of life | Inequalities
End of life | Inequalities
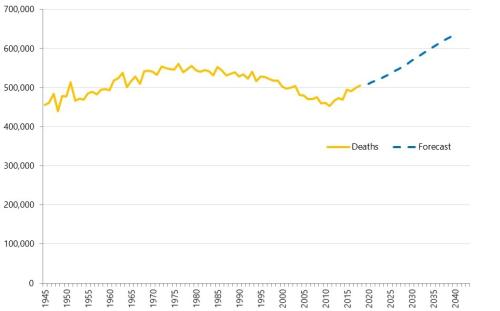
Health service use in the last two years of life
Health and care services get just one opportunity to support people at the end of their life. When this support is compassionate and appropriate, unnecessary suffering can be avoided and grieving can be eased. When this is not the case, harm and distress can result. The difference in these…
 Inequalities | Mental health
Inequalities | Mental health
Accessibility of perinatal mental health services for women from Ethnic Minority groups
Barriers to accessing mental health care during pregnancy and the first postnatal year (perinatal period) seem to be greater for ethnic minority women.
Modelling the impact of covid on waiting lists for planned care
Working with the national collaboration to coordinate covid-related analysis, and the NHSE/I Midlands region, the Strategy Unit has produced a ‘systems dynamics’ model of waiting lists for planned care. The model is freely available for non-commercial use across the NHS. Here, Steven Wyatt and Mike…
How can Integrated Care Systems collect and use more ‘person-centred intelligence’?
Working with our partners Ipsos MORI, we have produced detailed guidance and an offer of services to address this question. This webpage contains information about the work, and all the products from it. Please get in touch if you would like to improve your use of person-…
 Elective care | Emergency care | Finance and payments | Policy | Primary, community and social care services
Elective care | Emergency care | Finance and payments | Policy | Primary, community and social care services
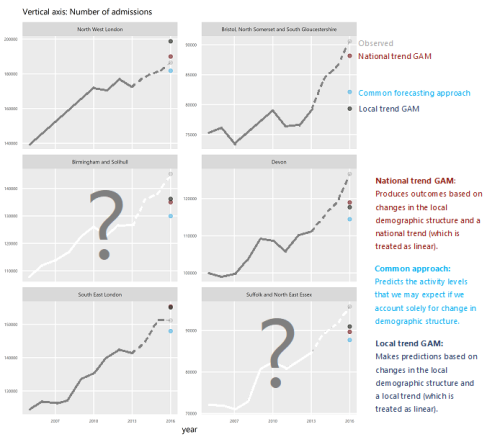
How will we know if Integrated Care Systems reduce demand for urgent care?
The implications of a blended payment system are far reaching: Decisions about planned activity levels will determine the total funding envelope for urgent care within a system and will influence the behaviour of healthcare providers and the services they deliver to patients.
 Emergency care | Policy
Emergency care | Policy
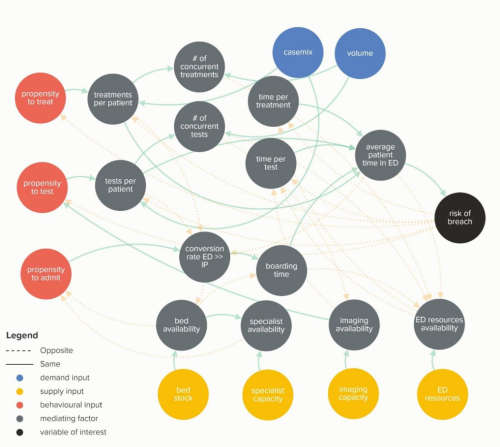
Waiting Times and Attendance Durations at English A&E Departments
In March 2019, NHS England is expected to report the outcome of its review of constitutional waiting times targets. This report reviews the factors that have led to the decline in performance against one of these targets - the 4-hour target for Accident and Emergency Departments. The analysis…
 Inequalities | Policy | Primary, community and social care services
Inequalities | Policy | Primary, community and social care services
New care models - what's the evidence
High level findings from a series of evidence reviews on new care models.
Risk and Reward Sharing for NHS Integrated Care Systems
Risk and reward sharing is a simple and attractive concept, offering a commissioner the opportunity to co-opt and incentivise a provider to moderate growth in healthcare demand by sharing in the savings or cost over-runs. The Centers for Medicare and Medicaid Services (CMS), a US government…