 Better use of analysis | Inequalities | Policy
Better use of analysis | Inequalities | Policy
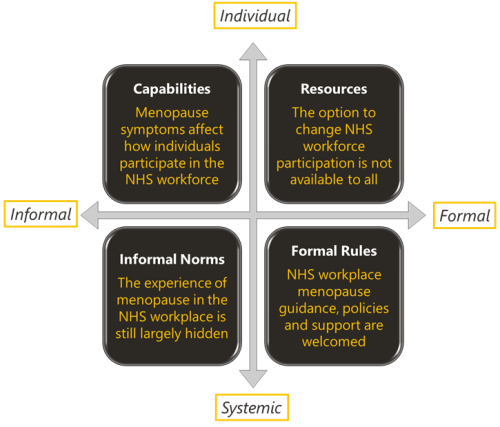
Menopause and the NHS workforce
The impact of the menopause on the NHS workforce. The Strategy Unit and Health Economics Unit report on their mixed methods findings.
 Better use of analysis | Elective care | Inequalities
Better use of analysis | Elective care | Inequalities
Inclusive Elective Care Recovery
These case studies present the key features and learning from local initiatives which championed inclusive approaches to elective care recovery.
 Secondary care | Service improvement
Secondary care | Service improvement
The NHS as an anchor institution: addressing fuel poverty
The number of households in fuel poverty in Staffordshire and Stoke-on-Trent (SSoT) is higher than the national average. As anchor institutions, NHS organisations can use their assets to influence the health and wellbeing of their local communities. The Strategy Unit was asked by the Midlands NHS…
 Better use of analysis | Inequalities
Better use of analysis | Inequalities
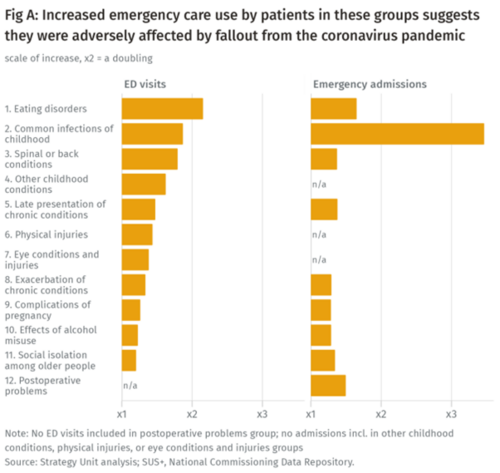
Population health implications of the Covid-19 pandemic
Our new report for The Midlands Decision Support Network (MDSN) presents findings of the effects of the care disruption, from the Covid-19 pandemic, on population health. The in-depth analysis identifies which patients and health conditions should be the focus of future efforts in reducing…
 Elective care | Inequalities | Policy
Elective care | Inequalities | Policy
What are the ethical challenges in addressing inequities?
Produced by Angie Hobbs - the world’s first Professor in the Public Understanding of Philosophy – this paper examines the ethical questions raised by our report outlining strategies for reducing inequity.
 Inequalities | Policy | Primary, community and social care services
Inequalities | Policy | Primary, community and social care services
Evaluation of Building the Right Support: Final Reports
Building the Right Support was a national plan to provide better support to people with a learning disability or autism.
 Mental health | Primary, community and social care services
Mental health | Primary, community and social care services
Inequities in children and young people’s mental health services
Good mental health during early years and childhood has a great bearing on health throughout life. By contrast, poor mental health can cast a long shadow. Consequences may include depression, self-harm, and poor physical health. Services recognise this. They aim to provide access to support in a…
 Better use of analysis | Elective care | Emergency care | Inequalities | Primary, community and social care services | Public health and prevention
Better use of analysis | Elective care | Emergency care | Inequalities | Primary, community and social care services | Public health and prevention
Less noise and more light: using criteria-driven analysis to tackle inequalities
Reducing health inequality is a long-standing aim of health policy. Yet the gap between policy aim and population outcome has grown in recent years: on most measures health inequalities have got worse.
 Elective care | Inequalities | Policy | Primary, community and social care services
Elective care | Inequalities | Policy | Primary, community and social care services
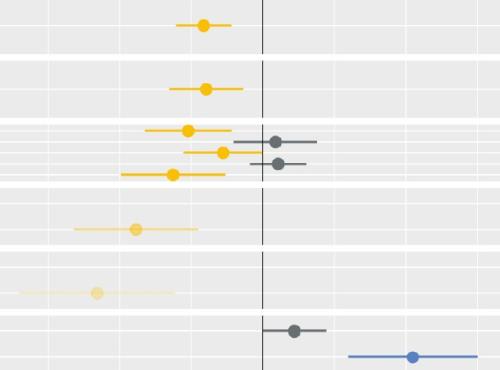
Socio-economic inequalities in access to planned hospital care: causes and consequences
Tacking inequalities in health is a long-standing NHS policy objective. Variation in the experiences and outcomes of different communities during the COVID-19 pandemic served to bring this issue back into focus.
 Elective care | Finance and payments | Inequalities
Elective care | Finance and payments | Inequalities
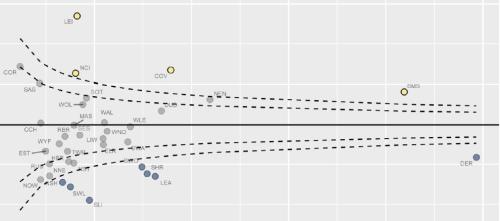
Equity and Cost Growth in Specialised Services
NHS specialised services provide care for people with complex or rare medical conditions. Treatments for these conditions are often expensive: While specialised services support a small proportion of the population, approximately one-sixth of the total NHS budget - over £19 billon - was allocated…
 Better use of analysis | Inequalities | Mental health
Better use of analysis | Inequalities | Mental health
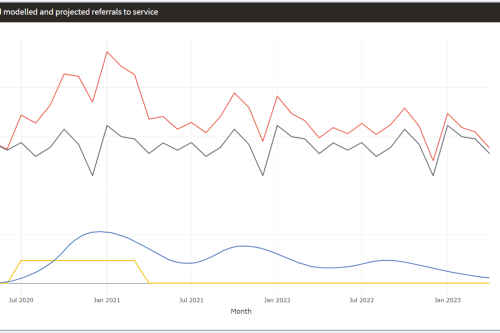
Mental Health Surge Model
Early in the Covid pandemic, it became clear that people’s mental health would suffer. Whether through bereavement, unemployment, social isolation, not being able to access support services – or a host of other routes – an alarming picture began to emerge and attract attention.
COVID-19: breaking the cycle of deprivation and ill health
Promoting whole-system action on the wider determinants of healthy life expectancy in the shadow of the COVID-19 pandemic
 End of life | Inequalities
End of life | Inequalities
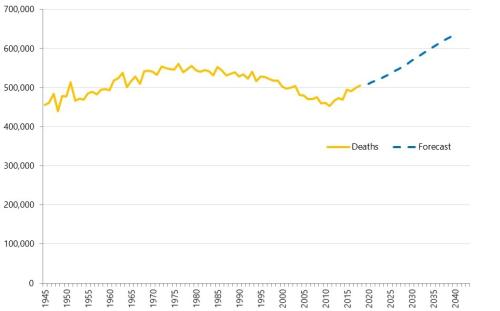
Health service use in the last two years of life
Health and care services get just one opportunity to support people at the end of their life. When this support is compassionate and appropriate, unnecessary suffering can be avoided and grieving can be eased. When this is not the case, harm and distress can result. The difference in these…
 Inequalities | Mental health
Inequalities | Mental health
Accessibility of perinatal mental health services for women from Ethnic Minority groups
Barriers to accessing mental health care during pregnancy and the first postnatal year (perinatal period) seem to be greater for ethnic minority women.
Modelling the impact of covid on waiting lists for planned care
Working with the national collaboration to coordinate covid-related analysis, and the NHSE/I Midlands region, the Strategy Unit has produced a ‘systems dynamics’ model of waiting lists for planned care. The model is freely available for non-commercial use across the NHS. Here, Steven Wyatt and Mike…
How can Integrated Care Systems collect and use more ‘person-centred intelligence’?
Working with our partners Ipsos MORI, we have produced detailed guidance and an offer of services to address this question. This webpage contains information about the work, and all the products from it. Please get in touch if you would like to improve your use of person-…
 Elective care | Emergency care | Finance and payments | Policy | Primary, community and social care services
Elective care | Emergency care | Finance and payments | Policy | Primary, community and social care services
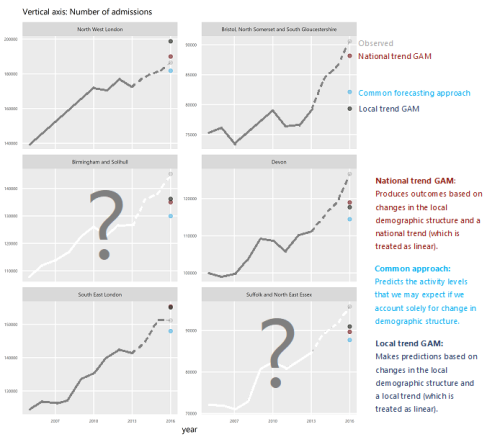
How will we know if Integrated Care Systems reduce demand for urgent care?
The implications of a blended payment system are far reaching: Decisions about planned activity levels will determine the total funding envelope for urgent care within a system and will influence the behaviour of healthcare providers and the services they deliver to patients.
 Elective care | Mental health
Elective care | Mental health
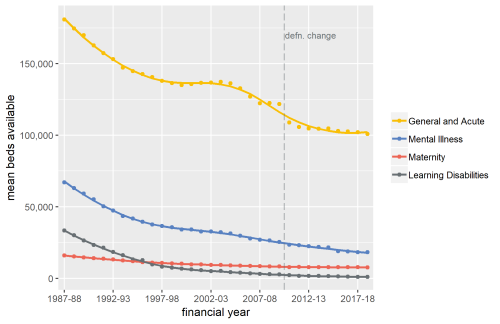
Exploring Mental Health Inpatient Capacity
This report explores the pressures on inpatient mental health services across Sustainability and Transformation Partnerships in England, drawing on a wide range of datasets, published research and interviews with staff working on mental health services. The report was commissioned by and includes…
 Inequalities | Mental health
Inequalities | Mental health
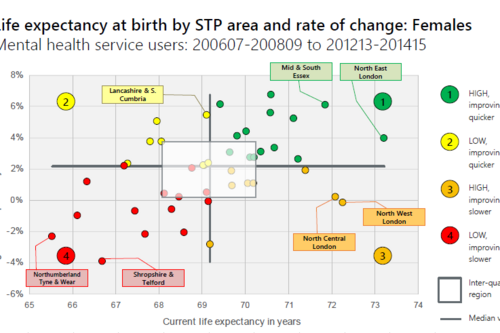
Making the case for integrating physical and mental health services in England - National overview
This is a national overview report of our Making the case for integrating physical and mental health services reporting which took place in July 2017. The original reports looked at the physical health of people who use mental health services; life expectancy, acute hospital use and…
Risk and Reward Sharing for NHS Integrated Care Systems
Risk and reward sharing is a simple and attractive concept, offering a commissioner the opportunity to co-opt and incentivise a provider to moderate growth in healthcare demand by sharing in the savings or cost over-runs. The Centers for Medicare and Medicaid Services (CMS), a US government…